
SUD COUNSELOR HANDBOOK
WITH DOCUMENTATION GUIDELINES
VERSION 3A
September 2020
Orange County Health Care Agency
Behavioral Health Services
Page 2 of 72
Contents
1. Introduction ..................................................................................................................................... 5
2. Medical Necessity............................................................................................................................ 5
ASAM & Levels of Care ..................................................................................................................... 6
Scope of Practice ................................................................................................................................. 8
3. Initial Assessment ............................................................................................................................ 9
4. Treatment Plan .............................................................................................................................. 16
Statement of the Problem ................................................................................................................... 17
Statement of the Goal ........................................................................................................................ 17
Action Steps ...................................................................................................................................... 18
Target Dates ...................................................................................................................................... 19
5. Continuing Services Justification & Treatment Plan Review .......................................................... 20
6. Progress Notes ............................................................................................................................... 23
OTHER COMPONENTS OF A PROGRESS NOTE: ........................................................................ 25
7. Codes & Services........................................................................................................................... 26
Withdrawal Management (WM) ........................................................................................................ 27
Billing Codes ................................................................................................................................. 27
Medication Assisted Treatment (MAT) .............................................................................................. 27
Billing Codes ................................................................................................................................. 27
Narcotic Treatment Programs/Opioid Treatment Programs (NTP/OTP) ............................................. 27
Billing Codes ................................................................................................................................. 27
Recovery Services ............................................................................................................................. 27
Billing Codes ................................................................................................................................. 27
Individual Counseling ........................................................................................................................ 28
Billing Codes ................................................................................................................................. 28
Assessment .................................................................................................................................... 29
Crisis Intervention ......................................................................................................................... 32
Treatment Planning ........................................................................................................................ 33
Collateral ....................................................................................................................................... 34
Family Therapy ............................................................................................................................. 34
Billing Codes ................................................................................................................................. 34
Individual Counseling .................................................................................................................... 35
Discharge Planning ........................................................................................................................ 36
Page 3 of 72
Case Management ............................................................................................................................. 37
Billing Codes ................................................................................................................................. 37
Group Counseling .............................................................................................................................. 40
Billing Codes ................................................................................................................................. 40
Billing ............................................................................................................................................... 43
NON-BILLABLE SERVICES: ...................................................................................................... 43
NON-COMPLIANT SERVICES ................................................................................................... 44
Time Reminders ............................................................................................................................ 44
8. Discharge Summary ....................................................................................................................... 44
9. Documentation Examples .............................................................................................................. 46
10. Appendix ................................................................................................................................... 48
Appendix A: Substance Use Disorder Diagnoses DSM-5 Criteria Guide ............................................ 48
Appendix B: ASAM Criteria Dimensions and Rationale Worksheet ................................................... 49
Appendix C: Documenting Impairments Related to SUD Guide ......................................................... 50
Appendix D: What Needs to be in The Case Formulation? ................................................................. 51
Appendix E: Billing Assessment and Re-Assessment Activities ......................................................... 53
Appendix F: Treatment Plan Reference Sheet .................................................................................... 55
Appendix F: What are SMART goals? ............................................................................................... 57
Appendix G: Treatment Plan Checklist .............................................................................................. 58
Appendix H: Sample Treatment Plan ................................................................................................. 59
Appendix I: Sample SUD Re-Assessment (Continuing Services Justification) .................................... 62
Appendix J: SUD Progress Note Checklist ......................................................................................... 67
Appendix K: Progress Note Elements ................................................................................................ 68
Appendix L: Documentation Language by Service Type .................................................................... 69
Appendix M: Sample Discharge Plan ................................................................................................. 70
Appendix N: Sample Discharge Summary ......................................................................................... 71
Page 4 of 72

Page 5 of 72
1. INTRODUCTION
PURPOSE
The County of Orange provides Substance Use Disorder (SUD) services to adolescents
and adults who have a substance use disorder.
The County of Orange has opted in to participate in the State’s Drug Medi-Cal Organized
Delivery System (DMC-ODS), which allows greater coordination of care for clients as they
move from one level of care to another, thereby increasing the likelihood of successful treatment
outcomes.
Participation in the DMC-ODS also means a new set of regulations that we must abide
by. Documentation is vital to maintaining a record of the quality of the services provided to
SUD clients. It is our responsibility to our clients to accurately describe the services provided,
which also includes the need to understand how to code services properly. This manual is
designed to help provide guidance on documentation standards to all clinical staff who work
directly with our clients in our SUD programs so that we may work towards maintaining
compliance with the regulations. It is intended to complement the documentation trainings
provided by Authority and Quality Improvement Services (AQIS).
Please note that this manual is for educational purposes only.
***DISCLAIMER***
This manual is a living document and will be amended as needed, based on changes made by the
State as well as any internal program requirements implemented. Please keep in mind that the
State sets the minimum requirements and the County can impose standards above and beyond the
State’s guidance. This current version is based on the current understanding of the State
regulations as well as the County’s agreement with the State on what will be provided.
2. MEDICAL NECESSITY
Medical necessity is the foundation on which all treatment rests. According to the DMC-ODS
standards, clients must meet the following medical necessity criteria:
1. Must have one diagnosis from the Diagnostic and Statistical Manual of Mental
Disorders (DSM-5) for Substance-Related and Addictive Disorders with the
exception of Tobacco-Related Disorders and Non-Substance-Related Disorders.
2. Must meet the American Society of Addiction Medicine (ASAM) Criteria definition
of medical necessity for services based on the ASAM Criteria.
3. If applicable, must meet the ASAM adolescent treatment criteria.
Clients who do not meet the full diagnostic criteria for a substance use disorder, cannot be
admitted into treatment. They may, however, qualify for the 0.5 ASAM Level of Care (Early
Intervention). Adolescents who may be “at risk” of developing a substance use disorder can be

Page 6 of 72
referred to receive Prevention & Early Intervention or other appropriate services through the
County. Adults can be referred back to the Beneficiary Access Line for resources.
ASAM & Levels of Care
The American Society of Addiction Medicine (ASAM) is a professional medical society, well
established in representing professionals in the field of addiction medicine. The ASAM focuses
on education, research, access, and improving the quality of treatment. The ASAM has
developed a comprehensive guideline for placement of individuals seeking and continuing
substance use treatment services, which is commonly referred to as the ASAM Criteria. The
ASAM Criteria has become the industry standard in the assessment and treatment of addiction.
Thus, it is one of the requirements of DMC-ODS.
The ASAM Criteria takes into consideration various factors of an individual’s life to help
streamline the determination of what level of care would be most appropriate. As we know,
there are many stages within recovery, and it is a fluid, lifelong process to maintain a sober
lifestyle for many of our clients. The ASAM Criteria offers to improve treatment outcomes by
accurately assessing the client’s needs and ensuring that the services provided meet those needs.
The client’s needs are assessed through each of the six (6) dimensions of the ASAM Criteria,
which are as follows:
1. Acute Intoxication and/or Withdrawal Potential
2. Biomedical Conditions and/or Complications
3. Emotional, Behavioral, and/or Cognitive Conditions and/or Complications
4. Readiness to Change
5. Relapse and/or Continued Use Potential
6. Recovery/Living Environment
Based on how severe the client’s functioning is in each of these six (6) dimensions, clients will
receive services at the corresponding levels of care. The ASAM Levels of Care are as follows:
Continuum of Care Services within DMC-ODS
Level 0.5
Early Intervention
Screening, Brief Intervention, and Referral to Treatment
(SBIRT)
Level 1.0
Outpatient Services
Less than 9 hours of service/week (adults);
Less than 6 hours of service/week (adolescents)
Level 2.1
Intensive Outpatient
Services
9 or more hours of service/week (adults);
6 or more hours of service/week
Level 2.5
Partial
Hospitalization
Services
20 or more hours of service/week (not requiring 24-hour
care)
Level 3.1
Clinically Managed
Low-Intensity
Residential
Treatment Services
24-hour structure with available trained personnel; at
least 5 hours of clinical service/week
Level 3.3
Clinically Managed
Population-Specific
24-hour care with trained counselors; less intense milieu
for those with cognitive or other impairments

Page 7 of 72
High-Intensity
Residential Services
Level 3.5
Clinically Managed
High-Intensity
Residential Services
24-hour care with trained counselors
Level 3.7
Medically
Monitored Intensive
Inpatient Services
24-hour nursing care with physician availability for
significant problems in Dimensions 1, 2, or 3; 16
hours/day counselor availability
Level 4
Medically Managed
Intensive Inpatient
Services
24-hour nursing care and daily physician care for severe,
unstable problems in Dimensions 1, 2, or 3; counseling
available to engage client in treatment
OTP
Opioid Treatment
Program
Daily or several times weekly opioid agonist medication
and counseling available to maintain multidimensional
stability for those with severe opioid use disorder
Withdrawal Services within DMC-ODS
Level 1-WM
Ambulatory withdrawal
management without
extended on-site monitoring
Mild withdrawal with daily or
less than daily outpatient
supervision
Level 2-WM
Ambulatory withdrawal
management with extended
on-site monitoring
Moderate withdrawal with all
day withdrawal management
and support and supervision;
at night has supportive family
or living situation.
Level 3.2-WM
Clinically managed
residential withdrawal
management
Moderate withdrawal, but
needs 24-hour support to
complete withdrawal
management and increase
likelihood of continuing
treatment or recovery.
Level 3.7-WM
Medically monitored
inpatient withdrawal
management
Severe withdrawal, needs 24-
hour nursing care &
physician visits; unlikely to
complete withdrawal
management without medical
monitoring.
Level 4-WM
Medically managed intensive
inpatient withdrawal
management
Severe, unstable withdrawal
and needs 24-hour nursing
care and daily physician visits
to modify withdrawal
management regimen and
manage medical instability.

Page 8 of 72
Scope of Practice
All staff are expected to provide treatment services within his or her scope of practice. An
individual’s scope of practice is dependent on education, training, and experience.
A “Licensed Practitioner of the Healing Arts,” or “LPHA,” includes: Physicians, Nurse
Practitioners, Physician Assistants, Registered Nurses, Registered Pharmacists, Licensed Clinical
Psychologist (LCP), Licensed Clinical Social Worker (LCSW), Licensed Professional Clinical
Counselor (LPCC), and Licensed Marriage and Family Therapist (LMFT) and licensed-eligible
practitioners working under the supervision of licensed clinicians. Those in the above disciplines
must also abide by the scope of practice guidelines set forth by the respective certifying or
licensing board.
Professional staff or “counselors” are either licensed, registered, certified, or recognized under
California State scope of practice statutes. This includes LPHA and those registered or certified
as an Alcohol and/or Drug (AOD) Counselor.
Trainees of a behavioral health discipline (those in graduate programs of study who may be
gaining internship or practicum hours in a SUD clinic) are not authorized to provide services in
the DMC-ODS. If a trainee is also registered as an AOD Counselor, he or she may provide and
bill for services in the DMC-ODS program working within the scope of a registered AOD
Counselor. Providers will need to keep in mind that the service and corresponding
documentation by this provider type must reflect the scope of practice of an AOD Counselor.
Please ensure that trainees are fully advised of the requirements and implications of registering
as an AOD Counselor. A registered AOD counselor “shall complete certification as an AOD
counselor within five (5) years of the date of registration” (CCR Title 9, Chapter 8, Subchapter 3,
Section 13035 (f)(1) and (2). Additionally, please be sure to confirm with graduate training
programs and administration in regards to the granting of credit for internship or practicum hours
intended to fulfill the requirements of a graduate program while the individual operates under a
different discipline.
The link below is a helpful grid provided by the State Department of Health Care Services
(DHCS) to clearly show what types of services are allowed to be provided and by whom:
http://www.dhcs.ca.gov/provgovpart/Documents/DMC-
ODS_Waiver/ODS_Staffing_Grid_Revised_031518_Final.pdf
DMC-ODS also requires that counselors and clinicians receive training in ASAM
Multidimensional Assessment and From Assessment to Service Planning and Level of Care, also
known as ASAM A and ASAM B prior to delivering DMC-ODS covered services. Training in
two (2) Evidence-Based Practices (EBP) is also required. In order to bill for services under
DMC-ODS, providers must complete all required training as shown on the DMC-ODS Training
requirements Policy and Procedure (P&P). This and all other BHS P&P can be found by visiting
www.ochealthinfo.com/bhs/pnp.
LPHA must obtain a minimum of five (5) hours of continuing education related to addiction
medicine each year.

Page 9 of 72
Physicians must obtain a minimum of five (5) hours of continuing medical education related to
addiction medicine each year.
3. INITIAL ASSESSMENT
For SUD services, the initial assessment that is completed upon the client’s admission to
treatment, is where the documentation of medical necessity begins. As with any standard
assessment, it is a compilation of information that is gathered from interviewing the client and, if
applicable, with information from significant others that may be involved with the client’s
treatment or referral for treatment. The assessment must include information about the following
aspects of the client’s life:
1. Drug and/or alcohol use history;
2. Medical history;
3. Family history;
4. Psychiatric/psychological history;
5. Social/recreational history;
6. Financial status/history;
7. Educational history;
8. Employment history;
9. Criminal history, legal status; and
10. Previous SUD treatment history
Since the initial assessment is where medical necessity must first be documented, the County’s
SUD Assessment form incorporates the six (6) dimensions of the ASAM Criteria. All of the
above information that must be incorporated into a standard assessment, is intended to be
addressed in the County’s SUD Assessment form through each of the dimensions. When using
the County’s SUD Assessment form, make sure that there is documentation for each of the ten
(10) elements listed above. It does not matter where the information is placed or in which
specific dimension, as long as it is included. For suggestions on where to place the required
assessment information in the County’s SUD Assessment, see the table beginning on page 10. It
is important to ensure all elements are included because missing information will result in
disallowance of services.
As we get to know our clients during the assessment period, we should always keep the
following in mind:
“How does this relate to the substance use?”
This is because we need to demonstrate how the problems in the client’s life is a result of the
substance use. These are the problems that we will be addressing in the client’s treatment.
Therefore, what is relevant to the substance use is what we need to clearly document. So, for the
purposes of our initial assessment, it is not enough just to gather information about the client’s
life. It is a purposeful gathering of information, directed at identifying how the substance use has
affected the client.
Page 10 of 72
With the information gathered, we must first determine whether the client meets the DSM-5
criteria for a substance use disorder. It is important to keep in mind the criteria for a substance
use disorder that can be our guide for the questions that we ask the client during the assessment.
It is not enough to say that since Johnnie has been drinking every night for the past 2 years, that
he has an Alcohol Use Disorder. Use alone is not enough to warrant a diagnosis. We must
identify the impact of the substance use. For a quick guide to the DSM-5 criteria for a substance
use disorder, refer to Appendix A (Page 48). Please remember that the non-LPHA cannot
diagnose the client. What the non-LPHA will be doing is gathering the necessary information so
that the LPHA can determine the most appropriate diagnosis. Therefore, the County’s SUD
Assessment form has two parts: pages 1-10 (Dimensions 1-6 and the Placement Summary),
which can be completed by either a non-LPHA or LPHA; pages 11-12 (Diagnosis and Case
Formulation), which can only be completed by the LPHA.
Diagnosis Required for Billing
Since the State requires a diagnosis for billing, this can present challenges for those situations
where the non-LPHA has conducted assessment sessions with the client and is going to bill for
those services. In such cases, the non-LPHA and an LPHA would need to consult so that the
LPHA can determine a diagnosis to be used for the purposes of billing. (This consultation is
different than the non-LPHA and LPHA consult for the creation of the Case Formulation or
establishment of medical necessity by the LPHA. For more information on the consultation
needed for the Case Formulation, see page 15 under “Important Reminders about the SUD
Assessment Form.”) The consultation for determining a preliminary diagnosis will need to take
place within the first three (3) days from the client’s admission to treatment or before the next
service, whichever comes first. Best practice would be to complete this consultation the same
day as the client’s admission. The consultation should be documented in the client’s chart to
demonstrate that it was the LPHA who provided the temporary diagnosis and not the non-LPHA.
This consultation is a billable Case Management activity and both the non-LPHA and the LPHA
can bill. The start and end time of the consultation needs to match for each of the progress notes
completed. If both parties are not going to bill, at minimum, the LPHA must document so there
is evidence of the LPHA determining the initial diagnosis for billing.
Below is a table showing how each of the above information that needs to be included in a
standard SUD assessment would fall within the County’s SUD Assessment form, as well as
where information related to the DSM-5 criteria can be included:
ASAM Criteria
Dimensions:
Required Assessment
Information:
DSM-5 Criteria for SUD
Diagnosis:
Dimension 1 – Acute
Intoxication and/or
Withdrawal Potential
• Drug and/or alcohol use
history;
• Previous SUD treatment
history
• Tolerance
• Needing to use more
to get the same effect
• Using the same
amount but not
getting the same
effect

Page 11 of 72
• Using more or for
longer than
anticipated
• Withdrawal
Dimension 2 – Biomedical
Conditions and/or
Complications
• Medical history
• Keep using even
when it is physically
dangerous to do so
• Keep using even
though the client
knows that there are
physical problems
caused by or made
worse by the use
Dimension 3 – Emotional,
Behavioral, and/or
Cognitive Conditions
and/or Complications
• Psychiatric/psychological
history
• Keep using even
when it is
psychiatrically
dangerous to do so
• Keep using even
though the client
knows that there are
psychological
problems caused by
or made worse by the
use
Dimension 4 – Readiness to
Change
• Previous SUD treatment
history (as it relates to
motivation and
willingness for
treatment);
• Family history;
Social/recreational
history; Financial
status/history;
Educational history;
Employment history;
and/or Criminal history,
legal status (as it relates
to severity of problems
impacting desire to
change)
• Ongoing use
impacting work,
school, home;
interpersonal
problems
• Keep using despite
knowing it is causing
problems
• Desire to
discontinue, but
unable to
Dimension 5 – Relapse
and/or Continued Use
Potential
• Previous SUD treatment
history (as it relates to
occurrences of relapse)
• Desire to
discontinue, but
unable to
• Keep using despite
knowing it is causing

Page 12 of 72
problems or is a
danger
• Inability to tolerate
withdrawal (using to
avoid withdrawals)
Dimension 6 –
Recovery/Living
Environment
• Family history;
• Social/recreational
history;
• Financial status/history;
• Educational history;
• Employment history;
• Criminal history, legal
status
• School, work, home
situation that has
suffered as a result of
use
• Not following
through or taking
care of
responsibilities at
home, school, or
work because of use
• A lot of time and
energy going towards
trying to get, use, or
recover from the use
The SUD Assessment form or similar psychosocial assessment is required for every intake at a
new provider.
For a tool that can be used to identify client-specific information for each of the dimensions of
the ASAM Criteria, refer to Appendix B (Page 49).
Transitions in level of care within the same provider
For those clients who may transition from one level of care to another within the same provider,
the SUD Re-Assessment form completed at the former level of care (which substantiates the
need for a different level of care) can also act as the initial assessment for the new level of care
that the client is going into. In such cases, the SUD Re-Assessment form must fulfill the
requirements of an initial assessment. This means that the required assessment elements need to
be addressed (Drug and/or alcohol use history; Medical history; Family history;
Psychiatric/psychological history; Social/recreational history; Financial status/history;
Educational history; Employment history; Criminal history, legal status; and Previous SUD
treatment history. See page 9 for more on the required assessment elements.). You may
reference the Initial SUD Assessment, if the relevant information has been captured at that time
and it has not changed. You will still want to include updates to any information because
changes in functioning must also be considered for determining the client’s current risk in each
dimension. For example, information in Dimension 1 might read, “See client’s past drug/alcohol
use history in SUD Assessment dated 1/5/2020. Client has been able to abstain from alcohol use
(weekly negative drug testing) throughout time in ODF and has been sober for a total of 4
months. Client does not exhibit or endorse any intoxication or withdrawal symptoms.”

Page 13 of 72
For information that has not changed and is not impacting the client’s severity in functioning in a
particular dimension, this should be noted. For example, if there have been no changes to the
client’s highest level of education from the time of the initial assessment in ODF to admission in
Recovery Services, it may be documented as “No changes in client’s education since admission
to treatment. See client’s educational history in SUD Assessment dated 1/5/2020.”
Example: The Santa Ana Clinic has Intensive Outpatient Treatment (IOT), Outpatient Drug Free
(ODF), and Recovery Services. Client X currently attends ODF at Santa Ana Clinic. The
counselor completes the SUD Re-Assessment for client X, which indicates the client is ready for
a lower level of care. Client X may transition to Recovery Services at Santa Ana Clinic and the
same SUD Re-Assessment (from ODF) can be used as the assessment that substantiates the need
for Client X to receive services at the Recovery Services level. A new treatment plan should be
created based on the information captured in the SUD Re-Assessment form.
Note that the State does not consider a transition from IOT to ODF within the same provider as a
discharge. Therefore, an initial assessment or the use of an SUD Re-Assessment that documents
the client’s readiness for discharge from IOT and the need for ODF does not need to be used as
the initial assessment for ODF, since it is not considered a new admission. However, since it is a
change in level of care and the needs of the client have changed, there still needs to be
documentation of medical necessity and it is advised that an SUD Re-Assessment be used to
document this. This ensures that the provider has done due diligence in applying the ASAM
Criteria to confirm that the client is ready to be transitioned. It is also advised that the provider
use this opportunity to check to make sure that the required assessment information has been
captured in the initial SUD Assessment or subsequent Re-Assessments. If the information was
lacking or insufficient, it should be captured in a Re-Assessment to demonstrate that all of the
client’s psychosocial history was considered.
Note that for the County Integrated Records Information System (IRIS) billing system, the IOT
and ODF levels of care are considered two separate episodes of care (EOC). This requires an
administrative step to end one EOC and start the other.
Transitions in level of care across different providers
The State allows for using the same assessment document when a client transitions from one
provider to another. This means that the SUD Re-Assessment completed to justify the client’s
appropriateness for discharge from Provider A’s program can be used as the initial assessment
for substantiating the client’s admission to Provider B’s program. The assessment document that
is being carried over will need to contain all of the elements of an initial assessment in order to
be used for that purpose. These include: Drug and/or alcohol use history; Medical history;
Family history; Psychiatric/psychological history; Social/recreational history; Financial
status/history; Educational history; Employment history; Criminal history, legal status; and
Previous SUD treatment history - See page 9 for more on the required assessment elements. It
will be the responsibility of the receiving provider to thoroughly review the assessment
document that is received from the client’s previous provider. In addition to the required
elements of an assessment, the receiving provider will also need to make sure that the assessment

Page 14 of 72
document sufficiently establishes the client’s medical necessity for services at the new program.
The LPHA will need to make this determination based on the information contained within the
assessment document. Upon review, if the assessment document received does not contain the
necessary information, it is advised that a full assessment or SUD Assessment form be
completed to ensure that the requirements of an initial assessment are fully satisfied and to avoid
disallowances. Relevant information from the previous provider’s assessment document can be
referenced as appropriate.
The time spent by the receiving LPHA reviewing the information on the assessment document
that is received from the previous provider is a billable activity coded as Case Management. In
order to justify billing for the time, the LPHA needs to clearly describe what he or she did
(review the client’s previous provider’s SUD Re-Assessment), what the purpose for doing so was
(to determine the client’s appropriateness for the receiving provider’s program), and what the
results of this review are (what clinical determination was made based on the review).
For a quick guide on billing associated with review of documents, see Appendix E (page 53).
How to Document the Connection between Substance Use and the Impairment
Although you may write it however you like, one suggestion is to use the following formula:
“Due to client’s ________________ (symptoms of SUD), client _________________
(behaviors) resulting in ______________________ (impairment).”
As you can see, this structure clearly shows the connection between substance use and the
impairment or problem. It is important to remember that substance use alone cannot lead to the
impairment or problem. For example, Susie may be drinking alcohol all throughout the day, but
this fact alone does not lead to her job loss. Something occurred as a result of Susie drinking all
day. Perhaps she was caught drinking at work or was often showing up late for work or not
following through with her work assignments or getting into verbal altercations with her co-
workers. There is a behavior that results from the use that leads to the problem. Another way to
think about this is how actions lead to consequences.
These statements help to concisely document how the client meets medical necessity and is most
helpful to use in the Rationale sections of each dimension on the SUD Assessment form and the
Case Formulation section. If the above formula is utilized, please remember to tailor it with
details specific to each client so it is not the same template from client to client. Using the same
template information has the potential to be scrutinized as fraudulent and susceptible to
recoupment. For additional help on documenting how the substance use is related to the
impairments, refer to Appendix C (Page 50) for a quick guide. For a helpful guide on how to
write the Case Formulation, see Appendix D (Page 51). For further assistance in completing the
County’s SUD Assessment form, please refer to the Accompanying Guide.
Important Reminders about the SUD Assessment Form

Page 15 of 72
1. For Residential Treatment, it is to be completed and signed within three (3) calendar days
of the client’s admission.
2. For Intensive Outpatient and Outpatient Drug Free, it is to be completed and signed
within thirty (30) calendar days of the client’s admission.
3. The Immediate Needs, Dimensions 1-6, and the Placement Summary may be completed
by the non-LPHA counselor. The Case Formulation and Diagnosis must be completed by
an LPHA.
4. If the assessment is completed by a non-LPHA counselor, there must be a consultation
(by face-to-face, telehealth, or telephone) between the non-LPHA counselor and the
LPHA who will review the assessment. This interaction needs to be documented to show
evidence that this consultation took place. It can best be captured using a progress note.
Both the non-LPHA counselor and the LPHA can account for the time spent in the
consultation through a billable Case Management note. This means that if the
consultation took 23 minutes, both the non-LPHA and the LPHA can claim 23 minutes
on each of their progress notes. Please remember that this interaction must be a separate
activity from clinical supervision. Clinical supervision is not billable to DMC. Caution:
The start and end times for the consultation on each note must match! The LPHA must
then complete the Case Formulation and the Diagnosis section of the SUD Assessment
form. The LPHA must complete and sign this within thirty (30) calendar days of the
client’s admission. It is permissible for the LPHA to document that the consultation took
place within the Case Formulation in lieu of completing a progress note. However, if
there is no separate progress note documenting the consultation, this means that the time
spent in that consultation cannot be billed. For a guide on billing for Assessment and Re-
Assessment activities, see Appendix E (page 53).
5. If the LPHA is the one who is completing the entire assessment document (no non-LPHA
involvement), the LPHA does not need to complete the Counselor Recommendation
section of the assessment. The LPHA can indicate “N/A” or “See case formulation.” It
is advised that the LPHA sign the page that includes the counselor’s recommendation
since it will make it clear to an auditor who completed dimensions 1-6 and the placement
summary.
6. If the SUD Assessment form cannot be completed within the timeframe specified above,
the reason(s) should be documented in the progress notes. If the assessment is not
completed by the end of the required timeframe, all additional services after this point
must be coded as non-compliant (services cannot be billed without a valid assessment
and treatment plan in place beyond the timeframe). Once the assessment and treatment
plan are completed, billing can resume.
7. If the SUD Assessment form is completed over multiple sessions, the initials and date on
the particular page of the assessment that was worked on should match the date
documented on the progress note where it is indicated that it was worked on. This is to
show that what was stated as completed in the progress note was actually completed on
that date.
8. If it is discovered that a person conducting assessments has not completed ASAM A and
B trainings prior to providing the assessment services, then the entire assessment service,

Page 16 of 72
treatment plan and all subsequent services will be considered non-compliant and will be
disallowed. The corrective action would be to have someone else who has completed the
required training complete an assessment (at the point at which the issue is discovered)
and to put a treatment plan in place.
***DISCLAIMER***
Above timeframes are determined by the State as well as any internal program agreements
made between the County and the State. Please keep in mind that the State sets the minimum
requirements and the County can impose standards above and beyond the State’s guidance.
4. TREATMENT PLAN
Once the SUD Assessment form has been completed, you now have the basis for building the
client’s treatment plan. The treatment plan is the client’s roadmap for his or her time in the
current treatment episode or level of care. The risk ratings that are indicated for each dimension
of the SUD Assessment form will help you to identify and prioritize the areas that need to be
addressed in treatment. It is expected that all problems identified in the assessment are reflected
on the treatment plan. However, not all need to be addressed at once. We must take into account
what will be feasible for the client as well as what the priorities are for the client. In order to
develop a meaningful treatment plan, it must be a collaborative process that includes the input of
the client. In the progress note for the session in which you collaborated with the client on the
treatment planning process, it can be documented as to why a particular problem will or will not
be addressed on the treatment plan. Such problems or goals can be “deferred” for a later date.
Treatment plans completed before the assessment
Since the treatment plan must be completed based on the information on the assessment, any
treatment plans developed and signed prior to the assessment being completed, will not be valid.
This is true regardless of whether or not the non-LPHA or LPHA completes the assessment with
the client. The information needs to be documented in sequence. The client’s diagnoses are
required to be on the treatment plan, which means that the formal diagnoses need to be
confirmed by the LPHA and medical necessity established. The LPHA will need to complete the
Diagnosis and Case Formulation sections of the SUD Assessment PRIOR to the development of
the treatment plan! Please note that dates of signatures on the treatment plan before the
completion of the assessment will result in recoupment. Services provided based on a treatment
plan signed before the completion date of the assessment would be non-compliant and will be
recouped if found to be using a billable CPT code. In this circumstance, an updated treatment
plan would need to be completed and signed reflecting a date of service that is on or after the
date on which the assessment was completed. Services on and subsequent to this date could then
be compliant and be billed using compliant CPT codes.
The following are the four (4) required components of a treatment plan:
1. Statement of the Problem
Page 17 of 72
2. Statement of the Goal
3. Action Steps
4. Target Dates
Statement of the Problem
These are based on the dimensions where impairments were identified and areas that need to
have a corresponding goal on the treatment plan. Since treatment planning is a collaborative
process with the client, it is important to explore with the client what problems he or she would
like to resolve or what he or she is looking to achieve. Although broad, it should not be a
category such as “addiction” or “medical.” Be more descriptive to identify what the problems
within those categories are. What the client expresses may or may not be related to substance
use (“I want to be a rock star” versus “I want to get clean”). With a statement that seems
unrelated to substance use, it will then be our job to work with the client on breaking it down to
what corresponds with what have been identified as the key problems in the assessment process.
Statement of the Goal
The goal is the broken down, more manageable piece of the problem that we will address in this
treatment episode. So, given the identified problem that corresponds to the dimensions of the
ASAM Criteria within the SUD Assessment form, we will want to determine “what do we need
to work on first to get you to where you want to be?” Goals must be measurable and or
quantifiable. Therefore, it is recommended that goals be written in the SMART format:
1. S – Specific
a. Targets an observable behavior
i. Example: Using coping skills to manage triggers; completing tasks for
acquiring employment (ties back to what was in the assessment)
2. M – Measurable
a. Quantifiable with a baseline and target (how often is it happening now and where
do we want it to be?)
i. Example: …from 0x/day to 3x/day; …from 4x/month to 1x/month
3. A – Achievable
a. Is the client willing? Is the client able? Set them up for success
4. R – Realistic
a. Results-focused, does it fulfill the desired reason for having that goal; applicable;
worthwhile
5. T – Time-bound
a. Setting a period of time, specific to the client, when the goal will be worked on
and progress can be tracked, which helps both the counselor and the client stay on
course.
A formula for writing a goal statement such as the one below can be used as an option to guide
you:

Page 18 of 72
“In the next __________________ (timeframe), client will ______________________ (behavior
change desired) from _______________ to __________________ (baseline and target) in order
to ____________ (how it addresses the problem).”
For a reference on treatment planning, see Appendix F (Page 55).
For a quick guide on SMART goals, see Appendix F (Page 57).
Remember to check to see if the client needs a goal for obtaining a physical exam. All clients
who have not had a physical exam within the twelve (12) months prior to admission to treatment
must have a goal on the treatment plan to address this. This is required for ALL levels of care,
including Withdrawal Management and Recovery Services.
Likewise, if there are any medical or health concerns or conditions that necessitate coordination
of care, there must be a goal on the treatment plan to address this.
Regardless of whether it is a perinatal program or not, if the client is pregnant or postpartum, the
treatment plan must address the requirements for covered services under the Perinatal Treatment
Guidelines (i.e., addressing treatment and recovery services specific to pregnant and postpartum
women like relationships, sexual and physical abuse, and development of parenting skills;
mother/child habilitative and rehabilitative services; education to reduce harmful effects of
alcohol and drugs on the mother and child/fetus; coordination of ancillary services).
Action Steps
Action Steps are what the counselor and/or the client will do to work towards achieving the
identified goal. They need to include the type of service that will be provided and by whom so
that it is clear what service our program is capable of providing and is being authorized for
billing. It also needs to include the frequency of the service or how often it will be provided.
Action steps must be clinical and within the scope of practice of the individual who will be
providing the stated action. They should also be written with enough specificity to provide an
outside reader with a good idea of what will be provided. For example, saying that “The
counselor will provide individual counseling to help client manage cravings” is pretty vague. It
begs the question, “How will you help the client to do this?” The “how” is what distinguishes
the counselor from the layperson because the counselor can provide clinical interventions based
on his or her education and training on how to treat clients with a substance use disorder. A
better intervention would be, “The counselor will provide individual counseling 1x/week to
educate client on the physiological and psychological effects of addiction,” or “The counselor
will provide individual counseling 2x/month to help the client identify changes in thoughts,
feelings, and behaviors associated with the experience of cravings.”
A formula for writing an action step such as the one below can be used as an option to guide you:
“(WHO – counselor, staff, therapist, etc.) will provide (TYPE OF SERVICE – individual
counseling, case management, etc.) (FREQUENCY – 1x/week, 2x/month, etc.) in order to
(example of the TYPE OF INTERVENTION that will likely be used for this type of service).”

Page 19 of 72
Target Dates
The target date is the anticipated date of completion for the particular action step. If there are
multiple action steps to a goal on the treatment plan, there needs to be a target date associated
with each one. However, the target dates for all action steps may be the same date. The date
should be determined based on the particular action step and be specific to the needs of the
client. Therefore, we should be moving away from designating a target that corresponds to the
length of a program or how long we expect the client to stay in treatment. Some action steps will
be able to be achieved in a few weeks whereas some action steps may take several months.
Important Reminders about the Treatment Plan
1. For Residential Treatment, it is to be completed, signed, and dated by the primary
counselor (or creator of the treatment plan) within ten (10) calendar days of the client’s
admission.
2. For Intensive Outpatient and Outpatient Drug Free, it is to be completed, signed, and
dated by the primary counselor (or creator of the treatment plan) within thirty (30)
calendar days of the client’s admission.
3. For Residential Treatment, the client must review, sign, and date the treatment plan
within ten (10) calendar days of the client’s admission.
4. For Intensive Outpatient and Outpatient Drug Free, the client must review, sign, and date
the treatment plan within thirty (30) calendar days of the client’s admission.
5. If the client refuses to sign the treatment plan, it should be documented in the progress
note along with a plan for how to engage the client to participate in treatment. The
treatment plan can be valid with the counselor and LPHA’s signature alone, only if there
is documentation of the reason for the missing signature of the client.
6. If the treatment plan is completed by a non-LPHA counselor, the LPHA must review,
sign, and date this within fifteen (15) calendar days from the date of the counselor’s
signature. This applies for Residential, Intensive Outpatient, and Outpatient Drug Free
levels of care.
7. If the counselor completing and signing the treatment plan is not the assigned primary
counselor, the primary counselor’s name must be indicated on the treatment plan.
8. If the treatment plan cannot be completed within the timeframe specified above, the
reason(s) should be documented in the progress notes.
9. After day ten (10) (for Residential) and day thirty (30) (for Intensive Outpatient and
Outpatient Drug Free), if there is no valid treatment plan completed, services are non-
compliant until the treatment plan is completed. Once the treatment plan is complete,
services can be billed going forward from the date of completion.
10. In the cases where the treatment plan is created by a non-LPHA, if the LPHA does not
sign the treatment plan within fifteen (15) calendar days from the counselor’s signature,
services are non-compliant between day fifteen (15) and the date of the LPHA’s
signature.
11. The client’s diagnosis or diagnoses must be on the treatment plan and must match what
was indicated on the diagnosis section of the SUD Assessment form. The ICD-10 code is
only necessary for billing purposes, therefore, it is not required to have the ICD-10 code

Page 20 of 72
on the clinical documents. The DSM-5 descriptor is sufficient. If both the ICD-10 code
and the DSM-5 descriptor are written, it is important to ensure that the two match. If
they do not match, this is a potential deficiency that can result in recoupment for services.
***DISCLAIMER***
Above timeframes are determined by the State as well as any internal program agreements
made between the County and the State. Please keep in mind that the State sets the minimum
requirements and the County can impose standards above and beyond the State’s guidance.
For a treatment plan checklist, see Appendix G (Page 58).
To see a sample treatment plan, see Appendix H (Page 59).
5. CONTINUING SERVICES JUSTIFICATION & TREATMENT PLAN
REVIEW
As we know, treatment does not happen in a bubble. Life still happens and circumstances
change. All while the client is going through their own change process in respect to their
substance use. Clinically, we know that an assessment is not final once the treatment plan is
created. Assessment is ongoing. We want to continue to assess (i.e. re-assess) the client for
changes in need. This too is a part of individualizing services to the clients. For Residential
Treatment, Intensive Outpatient Treatment, and Outpatient Drug Free levels of care, the way that
this can be documented is through the County’s SUD Re-Assessment form. Although we are
looking at the client’s progress in treatment on a regular basis, we need to have documentation
that the client is being re-assessed using the ASAM Criteria. WHY? It is a quality check to
make sure that we are addressing the client’s needs, taking into consideration their progress or
lack of progress and any new issues that may have come up in their lives that may impact their
recovery. This documentation helps to show that we are in tune with how the client is doing and
what the client needs. Is it clinically appropriate for the client to continue on the course of
treatment he/she has been on? Or do we need to change our approach or maybe even the
program and level of care to meet the individual needs of the client? A re-assessment of a client
can happen at any point in time as clinically necessary. The State specifically refers to this type
of documentation for ongoing medical necessity of services as a Continuing Services
Justification.
WHEN DOES IT NEED TO BE DONE? For Intensive Outpatient and Outpatient Drug Free,
a Continuing Services Justification (CSJ) is required to be completed no sooner than five (5)
months and no later than six (6) months from the client’s admission to treatment. The County’s
SUD Re-Assessment form can be used as it will have a place to indicate whether the form is a
CSJ or a Re-Assessment. The CSJ is required every six (6) months from the date of admission.
If there is no CSJ completed between the fifth (5
th
) and sixth (6
th
) month of treatment, services
will be disallowed and result in recoupment.
For Residential Treatment, there is no requirement for a CSJ. However, the County requires a re-
assessment every thirty (30) calendar days from the date of admission. Thus, the first SUD Re-
Page 21 of 72
Assessment form will need to be completed thirty (30) calendar days from the date of the client’s
admission to treatment and every thirty (30) calendar days thereafter. If the County SUD Re-
Assessment form is used, the “Re-Assessment” box can be checked. If there is no change in
diagnosis or change in level of care, the Case Formulation does not need to be completed. The
LPHA can simply co-sign to demonstrate that the information has been reviewed and that the
LPHA is in agreement with the outcome of no change in diagnosis or level of care.
It is recommended that the LPHA drop a billable Case Management note for review of the
Treatment Plan and Re-Assessment completed by the non-LPHA, particularly noting if there
were no diagnosis and/or level of care change.
***DISCLAIMER***
Above timeframes are determined by the State as well as any internal program agreements made
between the County and the State. Please keep in mind that the State sets the minimum
requirements and the County can impose standards above and beyond the State’s guidance.
WHAT NEEDS TO BE IN THE CONTINUING SERVICES JUSTIFICATION? The CSJ
is required for the Intensive Outpatient and Outpatient Drug Free levels of care. The following
are the required elements for justifying continuing services for a client:
• Consideration of the client’s personal, medical, and substance use history. (If the
required assessment elements were not clearly documented in the initial assessment,
be sure to include it in the CSJ. See page 9 and 12 for more information on the
required assessment elements.)
• Whether the client has received a physical exam. If so, state that/if there is a copy
in the chart.
• Taking into account the client’s progress on treatment plan goals based on progress
note documentation.
• Consideration of the LPHA or counselor’s recommendations.
• Statement about the client’s prognosis.
If the SUD Re-Assessment form (for fulfilling the CSJ between the fifth [5
th
] and sixth [6
th
]
month), is completed by a non-LPHA counselor, the LPHA will need to review, document the
basis for the need of continued services, and sign to show that the client meets medical necessity
for the level of care indicated. No consultation is required for the Re-Assessment or Continuing
Services Justification. The non-LPHA and LPHA may have a consultation at their discretion and
would be able to bill for the time spent as Case Management if they choose to do so. If, upon
review of the SUD Re-Assessment, the LPHA finds that the client does not meet medical
necessity, the client will need to be discharged and arrangements made for alternative care or
resources. Or the situation may be that the client does not meet criteria for the current level of
care, in which case, arrangements will need to be made to transfer or refer the client to the
appropriate level of care. The Case Formulation for the CSJ will need to include information on
how the client continues to meet the diagnostic criteria for the substance use related diagnosis
based on DSM-5. The documentation of impairments should focus on reflecting the severity of
the impairments related to the SUD diagnosis that warrants the need for the level of care being
indicated for the client.

Page 22 of 72
If the client is appropriate for a different level of care and needs to be transitioned, a short period
of transition is permitted, as long as the documentation demonstrates the need for the services
provided during the transition period. For example, if case management is needed to coordinate
the transition, this can be billed even though the CSJ has indicated that the client is not
appropriate for the current level of care. We would want to make sure that the documentation
clearly shows the purpose of the case management and why it was necessary.
For those clients whose CSJ or SUD Re-Assessment may have indicated that there is no other
need for treatment at the current level of care (such as clients who have completed all treatment
goals for this level of care) it is not required that the client be immediately discharged upon
completion of the CSJ or SUD Re-Assessment. It would be permissible, for quality of care, to
provide clients with a few transition/termination services. Again, the services that are provided
once it is determined that the client is ready for discharge, should be documented with
information to support the need for that particular service and indicate that it is for the purpose of
successfully preparing the client for discharge and/or access to recovery services.
To see a sample Continuing Services Justification form, see Appendix I (page 62).
IS A TREATMENT PLAN UPDATE REQUIRED? Yes. There will need to be an updated
treatment plan every ninety (90) calendar days from the date of admission. The primary
counselor and the client will work together to review progress and discuss whether the goals are
still relevant or if modifications are needed. For example, if there is no progress made on a goal,
perhaps the frequency needs to be changed, interventions modified, and/or the target date re-set.
Or it may be more appropriate to create a brand new goal that will better serve the client. In
order to adequately update a client’s treatment plan, there inevitably will be more involved in the
discussion than just whether the client is or is not making progress. In addition to changes to the
existing goals, there also needs to be consideration for what is currently happening in the client’s
life. It is an informal assessment of the client’s current functioning so that we may take into
consideration any new issues or areas of concern that should be incorporated into the client’s
treatment going forward. This helps to ensure that we are providing a tailored treatment that
addresses the client’s needs appropriately. This should be clearly documented in your session
progress note. New signatures will need to be obtained to show that this was discussed and
collaborated on with the client. Once the counselor and the client establish an updated treatment
plan, it will need to be signed by the client within thirty (30) calendar days from the counselor’s
signature. If the client refuses to sign the treatment plan, this needs to be documented. We also
need to document what our plan is for trying to engage the client and get the signature in the
future.
For Residential Treatment, the SUD Re-Assessment form is to be completed thirty (30) calendar
days from the client’s admission to treatment date and every thirty (30) calendar days thereafter,
but the treatment plan update is only needed ninety (90) calendar days from the client’s
admission to treatment date and every ninety (90) calendar days thereafter.
Regardless of the level of care, if the update to the treatment plan is done by a non-LPHA
counselor, it must be reviewed by an LPHA to determine whether continuing services are

Page 23 of 72
medically necessary. If approved, the LPHA needs to sign the updated treatment plan within
fifteen (15) calendar days of the counselor’s signature.
WHAT IF THERE ARE MULTIPLE TREATMENT PLAN UPDATES WITH NO
CHANGES? It is possible that your client may have made little or no progress towards goals,
but we need to demonstrate that we have done our professional duty to consider what we may
need to do differently. It may be that the goal just needs minor adjustments like striving to
implement the use of two coping skills instead of five. Perhaps it is the same goal, but we need
to modify the action step for individual counseling to focus on addressing the strain in the
client’s relationship with their family of origin that is at the root of their substance use rather
than general education about healthy relationships in recovery. Or maybe we need to increase
the frequency of one-on-one sessions because there is now an additional stressor of having
moved to a new sober living, causing greater anxiety and ambivalence.
***DISCLAIMER***
Above timeframes are determined by the State as well as any internal program agreements made
between the County and the State. Please keep in mind that the State sets the minimum
requirements and the County can impose standards above and beyond the State’s minimum
requirements.
6. PROGRESS NOTES
Progress notes are required for services claimed. At the Residential Treatment level of care, a
weekly progress note can be completed to capture all claimed services for the week.
The GIRP format for progress note documentation is shown below. Please consult with your
county administrator for documentation styles indicated for your facility.
G
Goal
• Topic or purpose of the session
• Goal(s) from the treatment plan that will be addressed
in this session
I
Intervention
• Description of what the counselor did to help the
client towards the goal of the session and goal(s) on
the treatment plan
• Clinical, within the scope of practice of the individual
providing it
• Related to the SUD
• Incorporate relevant Evidence-Based Practices
R
Response
• Description of how the client responded to the
counselor’s interventions
•
Stay objective and state the facts
P
Plan
• Description of what will be addressed in the next
session

Page 24 of 72
• Can include any follow up that may be needed prior to
the next session and/or miscellaneous information
about stage of change, new problems, overall progress
toward treatment goals
Using the GIRP format, the following are required elements that need to be in the content of each
note:
1. Topic or purpose of the session or service
2. The date of the session and the start and end times (for session and documentation)
3. A description of the client’s progress toward the treatment plan goals
4. Whether the service was provided in-person, by telephone, or telehealth
5. If services were provided in the community, the location must be identified as well as an
explanation as to how the client’s confidentiality was protected in that setting
It is important that the start and end time of the session is to the minute. It should accurately
reflect the actual start and end time of the session. In addition to the start and end time for the
session, the start and end time of the documentation for the progress note also needs to be
indicated in the note. For example, the session with the client present may have been from
2:13pm to 3:02pm, while the documentation for the progress note may have been completed
from 5:06pm to 5:15pm. The start and end times for documentation time can be indicated in the
body of the progress note. The State places a great emphasis on start and end times because of
the history of fraud that has occurred throughout the state. Regulators will be referring to the
time to confirm that staff are not providing multiple services at the same time.
For weekly progress notes at the Residential Treatment level of care, the start and end time for
each group or service provided in the week must be included in the note.
See Appendix J (Page 67) for a helpful checklist on progress note requirements.
TEMPLATED CONTENT: IS COPY AND PASTE OK? No. Please be careful not to “copy
and paste” information from one progress note to another, meaning that one progress note looks
like a carbon copy of another progress note intended for a different day or different client. This
type of documentation is considered fraudulent and will result in recoupment and/or compliance
investigations. There may be times when you may do the same intervention with a client over
several sessions, but there should be an explanation as to the purpose and intent of doing so. It is
expected that each individual session progress note is specific to the service and to the client.
You may use the same intervention but in different ways or focusing on different components
depending on the client and his or her needs. Therefore, your documentation would need to
demonstrate this. It is acceptable to have a general outline of how you would like to structure
your progress notes, however, the information needs to be made specific to that client and
session.
MY GROUPS ARE ALWAYS 90 MINUTES AND SCHEDULED FROM 10:00AM –
11:30AM, DO I STILL HAVE TO PUT THE EXACT START AND END TIME? Yes.
Page 25 of 72
Even if all groups are scheduled for a specific length of time, the reality is that groups often do
not start on time or end on time. It is important to capture these variances as billing with the
same exact number of minutes for every group is going to be flagged by the State as needing
review. Just as auditors do not like to see content that appears to be a template for progress
notes, they do not like the times to be a template.
DO I HAVE TO WRITE DOWN EVERYTHING THAT HAPPENED IN THE SESSION?
No. We want to protect the client’s privacy and confidentiality so we do not need to write
everything that happened or was said. It is about quality over quantity. Remember that the
primary purpose of a progress note is to document the service provided. It is not only necessary
for maintaining a good clinical record according to standard practice, but also necessary for
reimbursement. It is a record of what we are doing to help the client make progress toward his or
her treatment goals. Therefore, it must tie back to the substance use and effectively show how
the service is necessary to address this. Medical necessity must be evident and should be the
focal point of the documentation. Keeping this in mind will help focus the content of the
progress notes and keep your notes clear and concise!
HOW MUCH TIME DO I HAVE TO GET MY PROGRESS NOTE DONE? Progress
notes must be completed and signed within seven (7) calendar days of the session. The date of
the session counts as day one (1) and anything written after the seventh (7
th
) day cannot be billed
to Medi-Cal. If a note is written and signed beyond the seven (7) days, the note will need to be
made non-compliant.
For Residential programs, clinical services must be documented within seven (7) calendar days
of the service in order for it to count towards the required number of clinical hours for the week.
*The required number of clinical service hours in the week for Residential levels of care are five
(5) hours. These include medically necessary individual and group counseling sessions (groups
cannot exceed twelve [12] participants).
OTHER COMPONENTS OF A PROGRESS NOTE:
Face-to-Face Minutes is time with the client, in person. If the session or service was provided
by telephone, there would be no face-to-face time.
Non-Face-to-Face Minutes is billable time spent on a service activity that does not include
interaction with the client. Time spent providing a service via telephone would also be
considered Non-Face-to-Face time. Sessions with other individuals involved in the client’s
treatment and do not include the client, such as Family Therapy without the client present, would
be Non-Face-to-Face time.
Example: Analyzing information to determine risk rating levels for the dimensions of the ASAM
Criteria outside of the session with the client. The time spent working on this is billable.
Service Minutes is the billable face-to-face and/or non-face-to-face time.
Example: 45 minutes of face-to-face time with the client in a session to obtain information on
family, educational/vocational, legal, and social history. 45 minutes of non-face-to-face time
spent after session, without the client, working on conceptualizing the level of risk for dimension

Page 26 of 72
6 of the ASAM Assessment. The service time would be 90 minutes, and the note would reflect
45 minutes of face-to-face time and 45 minutes of non-face-to-face time.
Documentation Minutes is the time it took to complete the progress note. This should never
exceed the length of the session and should correspond to what is reasonable in comparison to
the interventions provided. This does not include typing or writing speed. It also does not
include technical difficulties. If the computer freezes and it took 10 minutes to restart and get
back to the note, this time cannot be accounted for in the documentation time.
Travel Minutes is the time it takes to travel from one location to another to meet with the client
to provide a billable service. Transporting a client does not count for this. If solely transporting
a client from point A to point B, this time is non-billable (Medi-Cal will not reimburse for us to
simply drive a client places). However, if during the course of transporting the client from point
A to point B, some billable service is provided (such as discussing recent response to triggers and
use of coping skills), this is considered Service Minutes because a service was provided. It may
be helpful to think of travel time as time in the car without a client and transportation time as
time in the car with a client when there is no service being provided. This does not mean that if
5 minutes of counseling was provided during a 30 minute drive, we can bill all 30 minutes! Only
the time spent providing an actual service can be billed.
• Billable Travel Time is time that can be billed when providing a billable service.
• Non-Billable Travel Time is when billable services are not provided or if solely
transporting the client (e.g., picking up a client to take to a doctor appointment).
For a guide on these other elements of a progress note, see Appendix K (page 68).
For a reference sheet on documentation language, refer to Appendix L (Page 69).
7. CODES & SERVICES
In this next section, we will take a look at the different codes that correspond to the type of
service that can be provided. Broadly, the services we provide to our SUD clients fall under
either individual counseling, case management, or group counseling.
DOES THIS MEAN THAT I CAN’T BILL FOR SERVICES IF I HAVEN’T CREATED
THE TREATMENT PLAN YET? No. In order to truly attend to the individual client’s needs,
there will be times when services need to be provided to the client before his or her treatment
plan is created (or during the thirty [30] calendar day window between admission to treatment
and when the treatment plan is due for an outpatient program, for example). In such cases, the
services can be billable as long as the documentation for that service justifies medical necessity.
In other words, the progress note for that session or service will need to show how that service
was necessary for addressing the client’s SUD and impairments. This is only during the
timeframe that the State allows for treatment plan development. For Residential Treatment,
since the treatment plan is due within ten (10) calendar days of the client’s admission, if medical
necessity is demonstrated, services prior to the ten (10) calendar days can be billed without a

Page 27 of 72
valid treatment plan. However, if there is no valid treatment plan after the ten (10) calendar
days, services must be coded as non-compliant until the treatment plan is complete. Once the
treatment plan is complete, services can be billed going forward. This will also apply for
Intensive Outpatient and Outpatient Drug Free, where the treatment plan is due within thirty (30)
calendar days of the client’s admission. If there is no valid treatment plan in place, services
billed after day thirty (30) must be made non-compliant until there is a valid treatment plan in
place. Once there is a valid treatment, services going forward can be billed.
Withdrawal Management (WM)
Billing Codes
Withdrawal Management (WM)
Level of Care/Service Type:
CDM/CPT Code:
WM Residential 3.2
99499-779
Medication Assisted Treatment (MAT)
Billing Codes
Medication Assisted Treatment (MAT)
Level of Care/Service Type:
CDM/CPT Code:
IOT MAT
99499-506
ODF MAT
99499-500
IOT MAT Vivitrol Administration (per dose)
90899-713
ODF MAT Vivitrol Administration (per dose)
90899-707
**All other billing within MAT falls under IOT/ODF services
Narcotic Treatment Programs/Opioid Treatment Programs (NTP/OTP)
Billing Codes
NTP/OTP
Level of Care/Service Type:
CDM/CPT Code:
OTP/NTP Methadone Dosing
90899-632
OTP/NTP Individual Counseling
90899-620
Recovery Services
Billing Codes
Recovery Services
Level of Care/Service Type:
CDM/CPT Code:
Residential 3.5 Recovery Monitoring
90899-689

Page 28 of 72
Residential 3.5 Perinatal Services Recovery
Monitoring
90899-776
Residential 3.1 Recovery Monitoring
90899-653
Residential 3.1 Perinatal Services Recovery
Monitoring
90899-671
IOT Perinatal Services Recovery Monitoring
90899-605
ODF Recovery Monitoring
90899-524
ODF Perinatal Services Recovery Monitoring
90899-551
Individual Counseling
Billing Codes
Residential
(billed by the day – includes individual/group counseling)
Level of Care/Type of Service:
CDM/CPT Code:
Residential Services 3.5
90899-674
Residential Services 3.1
90899-638
Intensive Outpatient
Level of Care/Type of Service:
CDM/CPT Code:
IOT Individual Intake
90899-554
IOT Individual Counseling
90899-560
IOT Perinatal Services Individual Intake
90899-581
IOT Perinatal Services Individual Counseling
90899-587
IOT Perinatal Recovery Services Individual
Counseling
50899-596
Outpatient Drug Free
Level of Care/Type of Service:
CDM/CPT Code:
ODF Individual Intake
90899-500
ODF Individual Counseling
90899-506
ODF Recovery Services Individual Counseling
90899-515
ODF Perinatal Services Individual Intake
90899-530
ODF Perinatal Services Individual Counseling
90899-533
ODF Perinatal Recovery Services Individual
Counseling
90899-542
Page 29 of 72
The Individual Counseling category is very broad and captures several different types of
activities or sub-categories:
1. Assessment
2. Crisis Intervention
3. Treatment Planning
4. Collateral
5. Family Therapy
6. Individual Counseling
7. Discharge Planning
Individual Counseling services can be provided in-person, by telephone, or by telehealth (except
in the case of assessment, which must be completed in-person or by telehealth).
Assessment
The following are billable assessment activities:
• Gathering psychosocial information for the SUD Assessment
• Interviewing the client about his or her substance use and its impact on functioning
• Formulating a DSM-5 diagnosis
• Determining the appropriate level of care
• Applicable for SUD Re-Assessment and Continuing Services Justification
I HAVE TO WRITE A LOT FOR THE ASSESSMENT, CAN I BILL FOR THAT? We
cannot bill for simply “completing the SUD Assessment form,” so we would want to avoid
words like “writing” or “typing” that may make it sound like we are doing the clerical aspect of
the assessment. Clerical tasks are not billable to Medi-Cal. The “completing” of the SUD
Assessment form needs to show that it took a counselor to do this and that some level of clinical
judgment was required. Therefore, we want to use words like “formulating,” “synthesizing,”
“conceptualizing,” etc.
This assessment formulation can be documented as non-face-to-face time (with zero face-to-face
minutes if client was not present) on a billable Individual Counseling progress note. If this
happens in conjunction with a session with the client, the time can be included in the session
note. For example, if 45 minutes was spent in a session with the client and then the counselor
spends 60 minutes working on determining the severity ratings and rationale for the client’s
impairments in each of the ASAM Criteria dimensions, this can be billed as one Individual
Counseling note with face-to-face time of 45 minutes and non-face-to-face time of 60 minutes.
For Residential levels of care, assessment activities that do not include the presence of the client
also fall under Individual Counseling. Since Individual Counseling is part of the daily bundled
rate for a residential program, it is included as part of what is offered by the program. This
means that it cannot be billed as an additional service for a residential program. Any non-face-
to-face time spent completing assessment activities should not be counted towards the required
Page 30 of 72
number of clinical hours for the week. Only activities that directly involve the client should be
counted.
MY CLIENT HAS A LOT OF PAPERWORK FROM OTHER AGENCIES THAT I
NEED TO REVIEW. CAN I BILL FOR MY TIME? If the activity is relevant to the client’s
treatment, it may be billable. Reviewing another document (i.e., discharge paperwork,
psychological evaluation, previous assessment, etc.) to help inform the assessment or treatment
plan would be billable as Case Management. Be sure to clearly document how the activity was
medically necessary.
The time spent by the LPHA to review the SUD Assessment completed by the non-LPHA as part
of determining the client’s diagnosis and medical necessity for services is billable as Case
Management. It can also be included in the time spent in the consultation with the non-LPHA (if
provided on the same day).
This is also applicable for the physician who may be reviewing physical exams. The time spent
reviewing can be billed as Case Management. It can also be included in the time the physician
spent providing consultation to staff about recommendations for follow up based on review of
the physical exams (if provided on the same day).
I WORKED ON THE ASSESSMENT OVER MULTIPLE SESSIONS. HOW DO I
DOCUMENT IT? Time spent working on analyzing and developing parts of the Assessment
form are billable. Here is where the initials and date on each page of the County’s SUD
Assessment form becomes important. If the counselor worked on Dimensions 1 and 2 on pages
2-4, the initials/date on those pages should match what is documented on the note. The
corresponding progress note may indicate, “This Counselor synthesized information to complete
Dimensions 1 and 2 (pages 2-4) on the SUD Assessment…” If the initials/date indicate those
pages were done on 11/11/17, then the corresponding progress note for 11/11/17 should
document the counselor’s work on this part of the assessment. Be sure to print out those
completed pages to place in the chart in the event that the chart is audited before the whole
assessment is completed. This is to help corroborate what the counselor is claiming to bill for
the activity and what is actually done. If the Assessment form is going to be completed in
sections, over a period of time, make sure that there is one clean copy placed in the chart once
completed. This is to help the auditor to be able to read through the assessment with ease and to
ensure all sections are in place. If the information was gathered over various sessions, the final
copy should be encompassing of all the information gathered up until the point of completion (in
which case all initials at the bottom of each page on that final copy will be dated the same date).
WHAT IF I HAVE NEW INFORMATION THAT THE CLIENT HAS GIVEN SINCE
THE INITIAL ASSESSMENT SESSION THAT I WANT TO ADD TO THE
ASSESSMENT FORM?
If those sections of the form were printed out to be placed in the chart (to demonstrate that the
time billed corresponds with what was worked on), the counselor should document this in the
session progress note to indicate that the assessment form will include updated information. The
counselor may then choose to manually add the information to the printed out pages (with
Page 31 of 72
initials/date of addition) or wait to include the new information or changes in the final, clean
copy of the Assessment form.
WHAT ABOUT ASSESSING FOR DANGER TO SELF (DTS), DANGER TO OTHERS
(DTO), AND GRAVE DISABILITY (GD)? Risk assessments, such as for DTS, DTO, and GD
do not fall under Assessment. Unless it was during a session where the counselor was working
on the assessment. In that case, the documentation for the risk assessment should be included in
the progress note for that assessment session or service. But the risk assessment alone does not
necessitate a separate document as an assessment note. For example, if during a regularly
scheduled Individual Counseling session, the client discloses thoughts about self-harm that
requires further evaluation to determine intent, means, and plan, it would be documented in the
Individual Counseling session progress note. Once your assessment is completed, follow your
agency’s protocol for addressing risks related to DTS, DTO, or GD.
Since assessment is ongoing and can be done at any point in the treatment process and applies to
all clients, the service does not need to be specifically identified on the treatment plan.
Assessment services can be provided in-person or by telehealth.
Note: For the initial assessment session where intake paperwork is provided, reviewed, and
signatures are obtained in order to enroll or admit the client into the program and the assessment
process is started, the CDM/CPT Code used will be for that labelled as “Intake.” This code is to
be used one time during the client’s episode of care. All other assessment sessions or activities
should be coded as “Individual Counseling.”
WHAT IS TELEHEALTH? A telehealth session means office or outpatient visits via
interactive audio and video telecommunication systems. Please refer to your program
administrator for the specific platform that is used for the interactive audio and video
telecommunication system at your site. We must have the client’s consent to receive services by
telehealth. Please be sure that there is documentation of the client’s consent. When using
telehealth to provide services, best practice is to make sure that the documentation includes
information about how the client’s confidentiality was ensured.
The ability to utilize telephone and telehealth as a means of providing services to our clients is
helpful for ensuring that clients stay connected and have access to the services that are needed.
Although services can be provided from anywhere in the community, both the client and the
provider must be in the state of California at the time the service is rendered. Those clients who
may need to temporarily be out of state for personal business cannot continue to receive
telephone and/or telehealth services while away. If clients are going to be out of state for over
thirty (30) calendar days, this does require that we discharge the client. The documentation
should clearly indicate that you have confirmed that the client is in California. The
documentation also should clearly show that the provider is in California as well.
DO WE NEED TO DO AN INTAKE NOTE? Yes, for all levels of care, there should be a
progress note completed for the intake session. For Intensive Outpatient Treatment and
Outpatient Drug Free levels of care, the “Intake” code should be utilized for billing this service.
This code is intended to be used one time for that initial session. For Residential levels of care,
there should be documentation of an intake session, even though there is no separate billing. The
Page 32 of 72
time spent with the client for the intake session can count towards the weekly clinical hours
required at Residential programs. Regardless of the level of care, the content for an intake note
should include information about how legal intake paperwork (i.e., informed consent, notice of
privacy practices, limits of confidentiality, etc.) was explained and reviewed with the client. It
should also include some assessment of the client’s appropriateness for treatment services (i.e.,
substance use history, referral source and reason, etc.). There should be enough assessment
information gathered to justify a working or provisional diagnosis until the full psychosocial
assessment or the SUD Assessment form can be completed.
Non-LPHA completing the intake service…Don’t forget that if the intake service is conducted
by a non-LPHA, there needs to be a consultation between the non-LPHA and LPHA so that a
working or preliminary diagnosis can be established for the purposes of billing (see page 9 for
more information on a diagnosis being required for billing).
Crisis Intervention
The following are billable crisis activities:
• Relapse
• Unforeseen event/circumstance presenting an imminent threat of relapse
The focus of the session or service is on alleviating the crisis problem and limited to the
stabilization of the client’s emergency situation. The above example of a client who discloses
thoughts of self-harm perhaps through overdose during a regularly scheduled Individual
Counseling session would constitute a crisis if it is determined that the client is at imminent
threat of relapse. If the counselor were to receive a phone call from the client who states that he
or she has just been kicked out of the home and is reporting thoughts and plans to relapse, this
would be considered a crisis situation. It would now require the counselor to stop what he or she
may be doing to address this situation and de-escalate the client to prevent relapse. Another type
of situation may be where the counselor is called out to the client’s place of residence because
the client has relapsed. The activities involved with obtaining information necessary to arrange
for potential medical attention and prevent ongoing use would be considered crisis intervention
activities.
DURING OUR SESSION, MY CLIENT DISCLOSES THOUGHTS OF HARM TO
OTHERS. IS THIS A CRISIS? Not necessarily. Thoughts of harm to others does not, by
itself, necessitate a crisis intervention. Additionally, since it happened during the course of a
regular session, the risk assessment is just a part of that session. Standard procedures for
assessing risk would be followed (i.e. determining the lethality based on whether there is intent, a
plan, and means). Obviously, if the client is truly a danger to others based on assessment, the
protocol for getting immediate help will need to be followed. If this is related to the substance
use because it poses “an imminent threat of relapse,” it is billable as crisis intervention.
“Imminent threat of relapse,” means that relapse is likely within the next few hours if there is no
intervention. If this is unrelated to substance use or a potential relapse (perhaps more mental
health related), the service would be non-billable. It does not mean that we cannot address the
issue; however, it will need to be coded accordingly.
Page 33 of 72
I WENT TO THE CLIENT’S HOUSE BECAUSE HIS MOM SAID HE WAS
RELAPSING, BUT WHEN I GOT THERE, HE WAS NOT. IS THIS STILL A CRISIS
NOTE? Crisis intervention can be billed up to the point that the counselor determines that the
situation is no longer a crisis because the intent of this service is to stabilize the situation. The
frantic call from the mother of the client, travel to the client’s home to address the potential
crisis, and the assessment to determine the nature of the crisis would be billed as crisis
intervention. Upon assessment of the client, where the counselor decides that the situation is no
longer a crisis (i.e. no actual relapse and/or no imminent threat of relapse), the billing for this
service would stop. Additional work done after this point (for example, speaking with the
mother and the client together to process the situation and work on effective communication
around potential relapse issues or triggers) would become a different type of service (in the prior
example, it would be a family counseling session). This can all be documented in one note, as
long as it falls under the same code. In the example above, it is a crisis (which falls under
Individual Counseling) until determined to no longer be a crisis, at which point family
counseling was provided (which also falls under Individual Counseling). Therefore, it can be
written in one note.
Crisis intervention does not need to be a service that is specifically authorized on the treatment
plan. However, we cannot bill for crisis (which is coded as Individual Counseling) without a
valid treatment plan in place once a signed treatment plan is already required to provide any
services. Instead, a non-compliant note should be written to document the crisis event and the
interventions provided as well as plans for completing/creating/updating a valid treatment plan.
Crisis intervention services can be provided in-person, by telephone, or by telehealth.
Treatment Planning
The following are billable treatment planning activities:
• Collaborating with the client on problems, goals, action steps, and target dates for the
treatment plan
• Developing an individualized treatment plan based on assessment information gathered
• Reviewing and/or updating the treatment plan goals
It will be helpful to think of determining needs and services as two different tasks. All
information related to addressing the needs of the client and what he or she will work on while in
treatment is considered treatment planning. The aspect of determining what services would best
accommodate those needs is considered case management.
Since treatment planning can happen at any time, even after a treatment plan has been
established, it does not require a specific authorization on the treatment plan.
Treatment planning services can be provided in-person, by telephone, or by telehealth.
As mentioned earlier in the Treatment Plan section, the collaboration with the client is an
important aspect. Therefore, it is important that there be documentation of a discussion with the
client about his or her treatment plan. Treatment planning sessions may be billed as Individual
Page 34 of 72
Counseling. (Please see page 16 for more information on completing treatment plans before the
assessment).
For Residential levels of care: treatment planning services fall under Individual Counseling,
which is part of the daily bundled rate. Time spent with the client working on treatment plan
development can be counted towards the required number of clinical hours needed each week.
In order for the time to count towards the clinical hours for the week, there must be
documentation on file to support that this service was provided.
Collateral
The following is a billable collateral activity:
• Sessions with significant people in the client’s life
Significant persons are those who have a personal, not official or professional, relationship with
the client. The focus of the session or service is on the treatment needs of the client and what
would support the client in achieving his or her treatment goals.
This is an activity that can be provided by AOD certified or registered counselors for any
psychoeducation or information gathered from significant people in the client’s life.
Collateral services can be provided in-person, by telephone, or by telehealth.
Collateral services can be provided with or without the presence of the client.
Billed as Individual Counseling with clear documentation of all parties involved in the service or
session.
For Residential levels of care: Collateral falls under Individual Counseling, which is part of the
daily bundled rate. Time spent providing Collateral services that includes the client can be
counted towards the required number of clinical hours needed each week. In order for the time
to count towards the clinical hours for the week, there must be documentation on file to support
that this service was provided.
Family Therapy
Although family therapy falls under the Individual Counseling category and gets billed as
Individual Counseling, we have separate CDM/CPT Codes internally to help distinguish this
documentation.
Billing Codes
MAT/Intensive Outpatient
Level of Care/Type of Service:
CDM/CPT Code:
IOT Family Therapy
90899-758
IOT Perinatal Services Family Therapy
90899-764
IOT Perinatal Recovery Services Family Therapy
90899-767
MAT/Outpatient Drug Free

Page 35 of 72
ODF Family Therapy
90899-746
ODF Recovery Services Family Therapy
90899-749
ODF Perinatal Services Family Therapy
90899-752
ODF Perinatal Recovery Services Family Therapy
90899-755
Only an LPHA working in their scope of practice can provide this service.
The following are billable family therapy activities:
• Family therapy brings the family into the treatment process to identify unhealthy family
dynamics that enable the addiction to continue. As unhealthy behaviors are identified,
families can then work on positive and healthy interactions with each other. Family
therapy can continue long after treatment is completed through referrals to licensed
practitioners. Family therapy is a self-discovery process for the entire family unit and
does not focus solely on the needs of the beneficiary.
Family therapy services can be provided in-person, by telephone, or by telehealth.
Family therapy services can be provided with or without the presence of the client.
Billed using the Family Therapy codes (which are billed to the State as Individual Counseling).
For Residential levels of care, Family Therapy falls under Individual Counseling and is part of
the daily bundled rate. However, time spent providing Family Therapy services that include the
client can count towards the required number of clinical hours needed each week. In order for
the time to count towards the clinical hours for the week, there must be documentation on file to
support that this service was provided.
WHAT IS THE DIFFERENCE BETWEEN COLLATERAL SESSIONS AND FAMILY
THERAPY? Collateral sessions involves counselors meeting with a client’s family or
significant others that can support their treatment needs. This service focuses on the treatment
needs of the client, and how loved ones can support the client during treatment and their
recovery process. These services are mostly educational or information gathering process.
Family therapy is a therapeutic process that can also address the needs of the family and the
larger, systemic issues contributing to the substance use or hindering the client’s recovery.
Individual Counseling
The following are billable individual counseling activities:
• Working with the client on skill-building for the purposes of maintaining sobriety and
relapse prevention
• Educating the client on issues related to substance use, such as concepts of withdrawal,
recovery, an alcohol and drug-free lifestyle
Page 36 of 72
• Increasing the client’s awareness and understanding about the recovery process and
utilization of supports like becoming familiar with related community resources
Interventions provided in an individual counseling session must be within the scope of practice
of the counselor providing the service. If Evidence-Based Practices (EBP’s) are referenced, it
should be clear how it is addressing the client’s treatment goals in order to individualize the
treatment to the needs of the client.
Individual counseling services can be provided in-person, by telephone, or by telehealth.
They are billed as Individual Counseling for the respective level of care that the client is
receiving.
For Residential levels of care, Individual Counseling services are part of the daily bundled rates,
but can count towards the required number of clinical hours needed each week. In order for the
time to count towards the clinical hours for the week, there must be documentation on file to
support that this service was provided.
Discharge Planning
The following are billable discharge planning activities:
• Collaborating with the client on creating the discharge plan
• Discussing plans for post-discharge and reintegration back into the community
• Preparing the client for referral into another level of care
Discharge planning services do not need to be specified on the treatment plan.
Discharge planning services can be provided in-person, by telephone, or by telehealth.
The session with the client where the discharge plan is collaborated on needs to be documented
to provide evidence that this occurred. This session is billable as an Individual Counseling
service.
For Residential levels of care: discharge planning falls under Individual Counseling and are part
of the daily bundled rates, but can count towards the required number of clinical hours needed
each week. In order for the time to count towards the clinical hours for the week, there must be
documentation on file to support that this service was provided.
If the service with the client involves discussing potential resources or referrals that are needed
upon discharge, this would be considered case management.
Discharge Plan
Except for those clients whose contact is lost, all clients will have a discharge plan.
The discharge plan can be completed by a non-LPHA or LPHA counselor. At minimum, it must
be completed within thirty (30) days prior to the scheduled date of the last face-to-face session
with the client. The discharge plan is a document that is to be worked on collaboratively with
the client. Again, if a counselor loses contact with the client (e.g., client being discharged due to

Page 37 of 72
client not showing up for sessions and being unable to be reached by phone, etc.), there is no
expectation that a discharge plan be completed.
The discharge plan must include, at minimum, the following information:
1. A description of the client’s relapse triggers
2. A plan to assist the client to avoid relapse when confronted with each trigger
3. A support plan (including referrals)
During the counselor’s last face-to-face session with the client, the counselor and the client will
need to sign and date the discharge plan. A copy must be provided to the client and the original
should be placed in the client’s chart.
DISCHARGE PLANNING STARTS AT ADMISSION! No matter the level of care the client is
at, the eventual goal is to help the client on his or her path to returning to the larger community
as a productive member without the need for the support of treatment services. Within each
level of care, we are working to help improve the client’s functioning enough to prepare the
client for the transition to a less restrictive setting. Therefore, as soon as the client enters
treatment, we should be looking at how we are going to help them transition out of treatment.
Working collaboratively with the client on this mentality will also serve to help the client
become more self-sufficient and avoid treatment dependence when the time does come for a
planned discharge. Additionally, the reality is that we never know when our last contact with our
client will be. The client may leave prematurely after two months of treatment or two days. It is
good practice to start the work of preparing for discharge in the early stages of treatment. It
should be an ongoing discussion and having a document that the client can reference is a great
tool for them.
For a sample discharge plan, see Appendix M, (page 70).
WHAT IS CONSIDERED A “LAST FACE-TO-FACE?” This must be a service that can be
entered into the County’s electronic health record and billing system (IRIS). Therefore, it must
be an activity that can be provided by a non-LPHA counselor or LPHA. This does not include
activities by Community Health Workers or front office staff. It also does not include drug
testing, regardless of who performs it. The service must be provided in-person.
Case Management
Billing Codes
NTP
Level of Care/Service Type:
CDM/CPT Code:
OTP/NTP Case Management
90899-611
WM
WM 3.2 Case Management
90899-782
Residential
Level of Care/Service Type:
CDM/CPT Code:
Residential 3.5 Case Management
90899-677

Page 38 of 72
Residential 3.5 Recovery Services Case
Management
90899-686
Residential 3.5 Perinatal Services Case
Management
90899-695
Residential 3.5 Perinatal Recovery Services
Case Management
90899-704
Residential 3.1 Case Management
90899-641
Residential 3.1 Recovery Services Case
Management
90899-650
Residential 3.1 Perinatal Services Case
Management
90899-659
Residential 3.1 Perinatal Recovery Services
Case Management
90899-668
MAT/Intensive Outpatient
Level of Care/Service Type:
CDM/CPT Code:
IOT Case Management
90899-569
IOT Perinatal Services Case Management
90899-593
IOT Perinatal Recovery Services Case
Management
90899-602
MAT/Outpatient Drug Free
ODF Case Management
90899-509
ODF Recovery Services Case Management
90899-521
ODF Perinatal Services Case Management
90899-539
ODF Perinatal Recovery Services Case
Management
90899-548
The following are billable case management activities:
• Assessment and reassessment of case management needs
• Transition to a higher or lower level of care
• Developing and/or revising services on a treatment plan
• Communication, coordination, referral activities
• Monitoring service delivery to ensure access
• Monitoring the client’s progress
• Advocacy and linkages to physical and/or mental health care, transportation, etc.

Page 39 of 72
The focus of case management is on the coordination of care for SUD and integration around
primary care. Our clients with a chronic substance use disorder and/or involvement with the
criminal justice system are likely going to need greater case management services.
Keep in mind that the case management needs must be related to the substance use in order for
the service to be billable to Medi-Cal. This will need to be clearly documented in the progress
note.
Case management services do need to be identified as a specific service on the treatment plan.
Case management services can be provided in-person, by telephone, or by telehealth.
Case management services can be provided with or without the client present.
Transitioning clients from one level of care to another
Case management services should be provided to assist with the transition to the next level of
care, while the client is still receiving treatment at the current level of care. We should not wait
to begin these case management activities until just prior to the client’s transition or until the
client is ready to move on. As a result, we are allowed a short transition period from the time the
client leaves the current level of care, for the purposes of continuity of care, to provide and bill
for case management. This period of transition should last no more than seven (7) calendar days
and corresponding documentation needs to justify each of the case management services
provided.
For the Residential levels of care, clients will be able to stay for forty-eight (48) hours after no
longer meeting medical necessity for that level of care, as long as it is for the purpose of
transitioning the person to the next level of care. There must be corresponding documentation
that explains the need for these extra days, and the client should continue to participate in
programming and case management services during the additional days.
Review of Documents
Case management can be billed by any level of care for time spent reviewing documents that are
pertinent to the client’s treatment. Please keep in mind that the amount of time claimed must be
supported by the documentation or explanation in the note. The explanation needs to include
what was reviewed and the purpose as well as its relevancy to the client’s overall treatment. If
the review of the document leads to a particular change or influences the course of treatment for
the client, this should also be captured in the documentation (see page 29 for more information).
Consultations
In addition to being able to bill for the consultation between a non-LPHA and LPHA for the
purposes of establishing a preliminary diagnosis or for completing the assessment process so the
LPHA can formalize the Case Formulation, there are other consultations that can be billed. Peer-
to-peer consultations within your agency may be a billable consultation. Oftentimes, there is a
need to coordinate the client’s care by discussing the client’s functioning and his or her needs
with others on your team. Most commonly this occurs for a primary counselor and a group

Page 40 of 72
facilitator to relay information about a possible change in behavior or need. In such instances, if
the consultation is a necessary activity that is relevant to the client’s treatment, it can be billed as
Case Management. As with other consultations discussed earlier, it can be billed by both parties
involved, as long as the start and end times match. In the documentation, it will be important to
clearly write the purpose of the consultation, who was involved, and how the exchange is related
to the client’s treatment. If the consultation or discussion leads to a change in course of
treatment or any actions that need to be taken to assist the client, this should also be noted.
Please be mindful that consultations that appear as appropriate for clinical supervision are not
billable.
Completing a Discharge Summary for Unplanned discharges
See page 44.
Group Counseling
Billing Codes
Residential
Level of Care/Service Type:
CDM/CPT Code:
3.1 Recovery Services Group Counseling
90899-647
3.5 Recovery Services Group Counseling
90899-683
MAT/Intensive Outpatient
Level of Care/Service Type:
CDM/CPT Code:
IOT Group Counseling
90899-563
IOT Perinatal Services Group Counseling
90899-590
IOT Perinatal Recovery Services Group
Counseling
90899-599
MAT/Outpatient Drug Free
ODF Group Counseling
90899-512
ODF Recovery Services Group Counseling
90899-518
ODF Perinatal Services Group Counseling
90899-536
ODF Perinatal Recovery Services Group
Counseling
90899-545
Group counseling services must be provided face-to-face with a minimum of two (2) and a
maximum of twelve (12) clients present in the group. One of those clients must be a Medi-Cal
beneficiary in order for the group to be billed to Medi-Cal. More than one therapist or counselor
is allowed in the group; however, this does not allow for changes to the maximum number of
clients allowed in the group or overall group billing amount.
Page 41 of 72
Groups will be limited to twelve (12) participants only. If it ever happens that a person is
overbooked and there are more than twelve (12) people present (even 1 extra), then it is
recommended that the program pull other staff and split up the group into 2 groups.
Alternatively, one client can be seen individually for a one-on-one session. This is because the
entire group would be non-compliant if it was run with more than twelve (12) clients present. As
usual, any non-Medi-Cal participants in the group will still count toward the twelve (12)
maximum and at least one (1) Medi-Cal client needs to be present. If this was found to be a
deficiency during reviews, the entire group would be disallowed and marked non-compliant.
Patient Education Groups are those groups that provide research based education on addiction,
treatment, recovery and associated health risks. Typically, these are conducted in lecture-style
formats. For the county clinics, an example of such a group is the HIV Education group offered
by a Registered Nurse at the Intensive Outpatient and Outpatient Drug Free levels of care. For
all levels of care, except Residential, Patient Education Groups cannot exceed twelve (12) people
in order to bill. If the Patient Education Group code is being used, please be sure that it is
billable only when there are two (2) to twelve (12) participants. At Residential levels of care, the
Patient Education Groups can exceed twelve (12) and will be counted as part of the structured
hours for the daily bundled rate.
For group sign-in sheets, please utilize one (1) sign-in sheet for all attendees in the group
(regardless of funding source). This is to demonstrate that the group size did not exceed the
maximum of twelve (12) allowed by DMC-ODS for billing. Clients should already be informed
during the intake process about confidentiality within the group setting. Please follow up with
your respective administrators for confirmation that this has been made explicit in the intake
paperwork. Some providers may choose to also include information on the actual sign-in sheets
to remind clients about this. It may also be helpful to review this with clients in the group setting
from time to time to ensure understanding.
Group counseling services do need to be identified as a specific service on the treatment plan.
Group services must be provided in-person.
For Residential levels of care: groups are part of the daily bundled rate. However, clinical
groups in a residential program can count towards the required number of clinical hours needed
each week.
WHAT NEEDS TO BE ON THE GROUP SIGN-IN SHEET? The printed name of the LPHA
or counselor conducting the group session must be on the group sign-in sheet. Next to the
printed name, the LPHA or counselor must provide his or her signature and date. The date of
signature should be the same as the date of the session. The LPHA or counselor is signing to
document that the information on the group sign-in sheet is accurate. The topic of the group,
date and start and end time of the group session must also be indicated on the group sign-in
sheet. Each participant will need to provide a signature with his or her full name printed on the
group sign-in sheet. If there is no corresponding group sign-in sheet to go along with the group
service documentation or progress note, the service cannot be billed.

Page 42 of 72
ARE ALL TYPES OF GROUPS BILLABLE? This depends on what the group is addressing.
According to the regulations, only “clinical” groups are billable to Medi-Cal. This means that
the group content must address a need related to the substance use that helps the client towards
achieving his or her treatment goals.
Groups such as house meeting would not be considered “clinical” groups. However, we know
that part of the purpose of the Residential setting is to provide structure for the clients to begin
learning and practicing sober life skills in a safe and contained environment. Therefore, if the
purpose is to build skills necessary to prepare for reintegration back into the larger community,
time spent on activities like chores, can be considered service hours that count towards the daily
required number of hours as long as it is clear on the documentation that such activities are
intended to build skills and not simply to occupy the client. It is helpful to focus on what the
intention of the activity is and ask ourselves, “how is this relevant to the client’s substance use
treatment?” and “how might this be beneficial for the client’s recovery?” and “what is the result
or benefit of the client participating in this activity?”
GROUP NOTE DOCUMENTATION
If the GIRP format is utilized for progress notes to document group services, the G (Goal) and I
(Intervention) section of the note may be the same across all participants in the group. This is
allowed because the group facilitator is providing the same intervention(s) to the entire group. It
is advised, however, that if the facilitator happens to provide an intervention to a particular
client, it should be documented on the progress note for that particular client. For example, if
one of the clients demonstrated a lack of engagement and there were prompts directed
specifically to that client, this can be noted in the I (Intervention) section to demonstrate how the
facilitator attempted to enhance the client’s participation. The R (Response) and P (Plan)
sections of the progress notes for the clients in attendance for that group will be specific to each
client, making each group note individualized to the client and to the service.
Please note that this does not mean that the I (Intervention) section of group service progress
notes can be the same across different groups. The interventions provided in the group setting
must be specific to that particular group. It needs to correspond with the topic of the group and
provide enough description of how the group topic was discussed to justify the amount of time
claimed. Groups are typically 60 or 90 minutes in length, so the interventions should reflect how
this time was used.
For the R (Response) section of the group service progress note, keep in mind that there should
be enough information to clearly illustrate how the client presented and behaved in the group.
Specifically, it is important to document the client’s reaction to the facilitator’s interventions.
For example, if the group topic was on improving communication and asserting one’s needs
effectively as a way to ask for help from one’s sober support network, the R (Response) section
should describe how the client did with this topic and the associated interventions. It will be
helpful to consider what the client may have said in the group or how he or she may have
Page 43 of 72
interacted with peers. Take note of how the client’s participation tells you that the client is or is
not making progress in treatment overall.
Billing
It is important for all services to be coded appropriately. In order to do this, we must understand
what services are not billable and when a chart is out of compliance (thereby not allowing us to
bill Medi-Cal).
NON-BILLABLE SERVICES:
Non-Billable services are defined as services that an outside third-party payer would NEVER
reimburse.
Activities considered by DMC to be services that are NOT billable can include but are not
limited to the following:
1. Waiting time
2. Translating/Interpreting
3. Clerical Services:
a. Faxing
b. Scheduling appointments
c. Photocopying
4. Searching for a missing client
5. Checking messages
6. Leaving messages
7. Providing transportation
8. Supervision with a supervisor/service chief
9. Completion of bus pass application
10. Completion of immigration form
11. Conducting internet searches
12. Most letter writing is not billable
13. Services for the sole purposes of addressing anything other than the substance use
disorder impairment. This can include solely dealing with:
a. Mental health and/or other excluded diagnoses
b. Health care
14. Any service while the client is in Jail/Juvenile Hall, Psychiatric Hospitalization, or an
Institute for Mental Disease (IMD)
a. Exceptions to this rule:
1. Day of admission
2. Placement services provided during the thirty (30) calendar days
immediately prior to the day of discharge for a maximum of three (3) non-
consecutive periods of thirty (30) days. These notes should be clearly
labeled “Placement Services.”
Rule of thumb: If the service you’re providing cannot be linked to the substance use or
impairments caused by the substance, it’s probably not billable.

Page 44 of 72
NON-COMPLIANT SERVICES
Non-Compliant services are defined as services that would normally be reimbursable but because
something is wrong with the chart (e.g., a failed treatment plan, late documentation, etc.) we are
not authorized to submit the services for billing. Additionally, services would be deemed non-
compliant if written after seven (7) calendar days or longer from the date of service.
A chart can be deemed out-of-compliance for several reasons. Most commonly, charts are out of
compliance due to a failed treatment plan. Treatment plans may fail for the following reasons:
1. Not signed by the client/conservator/legal guardian
(Exception: If the client refuses to sign, the treatment plan will still pass if documented
appropriately. However, mere refusal to sign because they don’t agree with the treatment plan is
not a sufficient reason).
2. Does not document medical necessity or show impairment related to the substance use
For a quick reference on billable vs. non-billable vs. non-compliant, see Appendix K (page 68).
Time Reminders
• Service minutes claimed must be substantiated by the interventions provided. Does the
documentation clearly reflect what took place in the session and the amount of time it
took to provide the service? Are we billing a 60 minute service for an activity that, as
documented, appears that it would take only a couple of minutes to do? Excessive
service minutes for what is documented may result in recoupment.
• Documentation minutes claimed must be congruent with the amount of the content
written. This is the only time that we are allowed to bill for an administrative function of
typing or writing. It must be a reasonable amount of time, meaning that an outside
observer would concur that the amount of the content would have taken the amount of
time that is being billed for documentation. Excessive documentation minutes for what is
documented may result in recoupment.
• As a general rule, documentation minutes should never be more than service minutes.
• Use actual minutes, not estimated time. Just as the start and end time for the service and
documentation must be exact and to the minute, rather than rounding to the nearest
quarter-hour or hour, the session or service times should reflect this as well. Using the
same standard amount of time for sessions (i.e., 50 minute individual counseling sessions
for all individual counseling sessions or 10 minute documentation for all progress notes)
is going to be a red flag that will necessitate a review of all of the corresponding
documentation.
8. DISCHARGE SUMMARY
Best practice is that for every client that is admitted, regardless of the length of stay and reason
for discharge, there will be a discharge summary completed.
However, at minimum, a discharge summary must be completed for every unplanned discharge.
The non-LPHA or LPHA counselor can complete it.

Page 45 of 72
The discharge summary must be completed within thirty (30) calendar days of the date of the last
face-to-face treatment contact with the client.
The discharge summary must include the following:
1. The client’s length of stay in treatment (date of admission to date of discharge)
2. Reason for discharge
3. Narrative summary of the treatment episode (include current alcohol/drug use,
vocational/educational achievements, transfers/referrals provided)
4. The client’s prognosis
Time spent on completing the documentation for the discharge of a client that is unplanned is a
billable Case Management service.
TYPE OF DISCHARGE
TYPE OF NOTE
Unplanned discharge
Billable Case Management
Planned discharge
Non-Billable Case Management
An unplanned discharge includes discharge due to loss of contact, the client leaving prematurely
against clinical advice such as “AWOL,” incarceration, abrupt move out of the area, etc. If there
was no opportunity to sit with the client to complete a discharge plan, due to the client leaving
the program earlier than expected, the completion of the discharge summary is a billable activity.
For transitions from one level of care to another within the same provider, the completion of the
discharge summary is not billable to DMC because it is not considered a discharge (see page 13
for more on transitions within the same provider). Please use the non-billable Case Management
code for completing the discharge summary and any additional discharge-related activities when
documenting. This is the administrative step required to end one EOC and to start another at a
different LOC.
For completing discharge summaries of unplanned discharges beyond the thirty (30) calendar
days from the last face-to-face with the client, do not bill Case Management. A non-compliant
code can be used for the progress note documenting the completion of the discharge summary in
such cases. Discharge summaries may only be billed as long as they occur within the required
thirty (30) days from that last service.
If using the County Discharge Summary form, please remember that the “Number of Minutes to
Complete the Discharge Process” is equivalent to Service Minutes. This is the time it takes to
research the client’s chart for information to complete the treatment summary narrative and
complete any other aspects of closing a client’s case. Just as we need to justify the amount of
time claimed for any progress note with Service Minutes, we must also include a brief
explanation as to how the time was spent for “Number of Minutes to complete the Discharge
Process.” This can be included as part of the narrative section with the client’s treatment
summary. The “Documentation Minutes” will be the amount of time it takes to complete the
discharge summary (since the progress note is embedded into the form). The “Documentation

Page 46 of 72
Date” and the “Facility and EOC Discharge Date” should be the same since the chart will be
closed as of the last date of charting.
For a sample discharge summary, see Appendix N (page 71).
9. DOCUMENTATION EXAMPLES
Individual Counseling Progress Note:
G: Client seen today at the clinic to address her SUD symptoms (alcohol use) and how they
interfere with her being active in the community: socializing, working, shopping, etc.
I: Writer processed with client about ways to cope with her feeling “on edge” and restless due to
triggers of being in social situations and large crowds of people. Role played situations in which
client is able to manage triggers using visualization and relaxation techniques of deep breathing
and grounding. Encouraged her to continue to practice applying these skills at least 2 times per
day so that when she is presented with a trigger, she can readily access techniques.
R: Client was able to process about possible coping skills with some prompting. As the session
progressed she became more at ease and showed reduced psychomotor agitation (stopped
tapping foot). She seemed to enjoy the role play and stated that she likes noticing “feeling
lighter” after using the relaxation techniques of deep breathing and grounding. Client initially
expressed low confidence in her abilities to utilize techniques on her own, but agreed that
regularly practicing them outside of the moments when she is triggered will help her to use them
more easily.
P: Client will continue to practice coping skills 2 times per day. Next session to follow up on her
independent use of coping skills as well as to process any actual instances of being triggered and
how it is managed. Client seems to be gaining more self-awareness and making slight progress
towards her treatment plan goal to increase use of coping skills to manage triggers.
Case Management Service Progress Note:
G: To meet with the sober living manager in an effort to coordinate services to help client to
improve relationships with other residents and prevent loss of housing that could threaten
recovery efforts.
I: Spoke with sober living manager about client’s recent verbal altercation with another resident.
Also inquired about his general observations of client’s behaviors and potential risks to sobriety.
R: Client was not present for this service. Sober living manager reported that client is
particularly agitated around one of the residents and sees that he often avoids interacting with
him. He acknowledged that he does need to intervene at times to prevent escalation of conflicts
between the two, but on most recent encounter, client seemed to be instigating. Sober living
manager expressed frustration with client and possibility that he may not be a good fit for the
house. Sober living manager shared that client seems to need help managing his anger and
impulsivity, saying that he has some concern that these may prompt client to return to using.
Page 47 of 72
P: Follow up with sober living manager over the next few weeks for monitoring of changes in
client’s behaviors and interactions with peers. Plan for next session with client is to develop
strategies for maintaining a conflict-free home environment and discuss its benefits to his
recovery. Coordination of care continues to be needed to help client make progress towards his
treatment goal to reduce altercations with others that perpetuate behaviors associated with use.
Group Counseling Service Progress Note:
G: To encourage discussion around the behavior of lying during substance use and allow the
group to reflect on its effects and what it means to live a more honest life in order to help client
maintain sobriety.
I: This writer explored with the group the importance of honesty in recovery. The group was
encouraged to give input on what honesty in recovery means for them. This writer discussed
how lying is a significant behavior in the life of an individual using substances and how it
evolves over time. This writer helped normalize common thoughts and feelings surrounding the
act of lying during use and how it changes with the stopping of use. Group members were asked
to share personal experiences of what has helped them to break out of the cycle of lying after use
and manage feelings of guilt that may remain after use has stopped. In closing, this writer had
group members identify what new opportunities and positive outcomes have come about from
embracing honesty in their recovery journey.
R: Client was more withdrawn in this session than usual, but participated with prompting. Client
was able to share that he continues to feel guilty for lying to his family during his use. Client
seemed to be listening and reflecting on what his peers shared. Client was more engaged
towards the end of the session and verbalized that he wished to continue to work on being honest
with himself and others, but that it was still difficult at times to face the feelings without using so
that he does not have to feel difficult emotions.
P: For client to continue to engage in groups and work towards increasing self-awareness and
verbalization of thoughts and feelings. Client seems to be making adequate progress toward his
goal to effectively communicate his needs so that he does not bottle up emotions, which is a
prominent trigger for him to use.

Page 48 of 72
10. APPENDIX
Appendix A: Substance Use Disorder Diagnoses DSM-5 Criteria Guide
According to the DSM-5, it is a pattern of substance use that results in clinically significant impairment
(minimum of 2), within 12 months:
CRITERIA:
1. Substance is taken more or for longer than anticipated
2. Have wanted to use less or stop or have tried to, but could not
3. A lot of time and energy going towards trying to get, use, or recover
from the use
4. Craving to use
5. Not following through or taking care of responsibilities at home,
school, or work because of use
6. Keep using even though responsibilities at home, school, or work are
neglected
7. Less or stopped involvement in social, work, or pleasurable activities
8. Continuing to use even though there have been instances of it being
physically dangerous
9. Knowing that the use is causing physical or psychological problems,
but continuing anyway
10. Signs of tolerance – needing more than you used to in order to get the
same feeling OR using the same amount you used to does not achieve
the effect it used to
11. Signs of withdrawal – specific to substance or substance is taken to
avoid withdrawal
TOTAL:
Mild = 2-3 of the criteria are met
Moderate = 4-5 of the criteria are met
Severe = 6 or more of the criteria are met
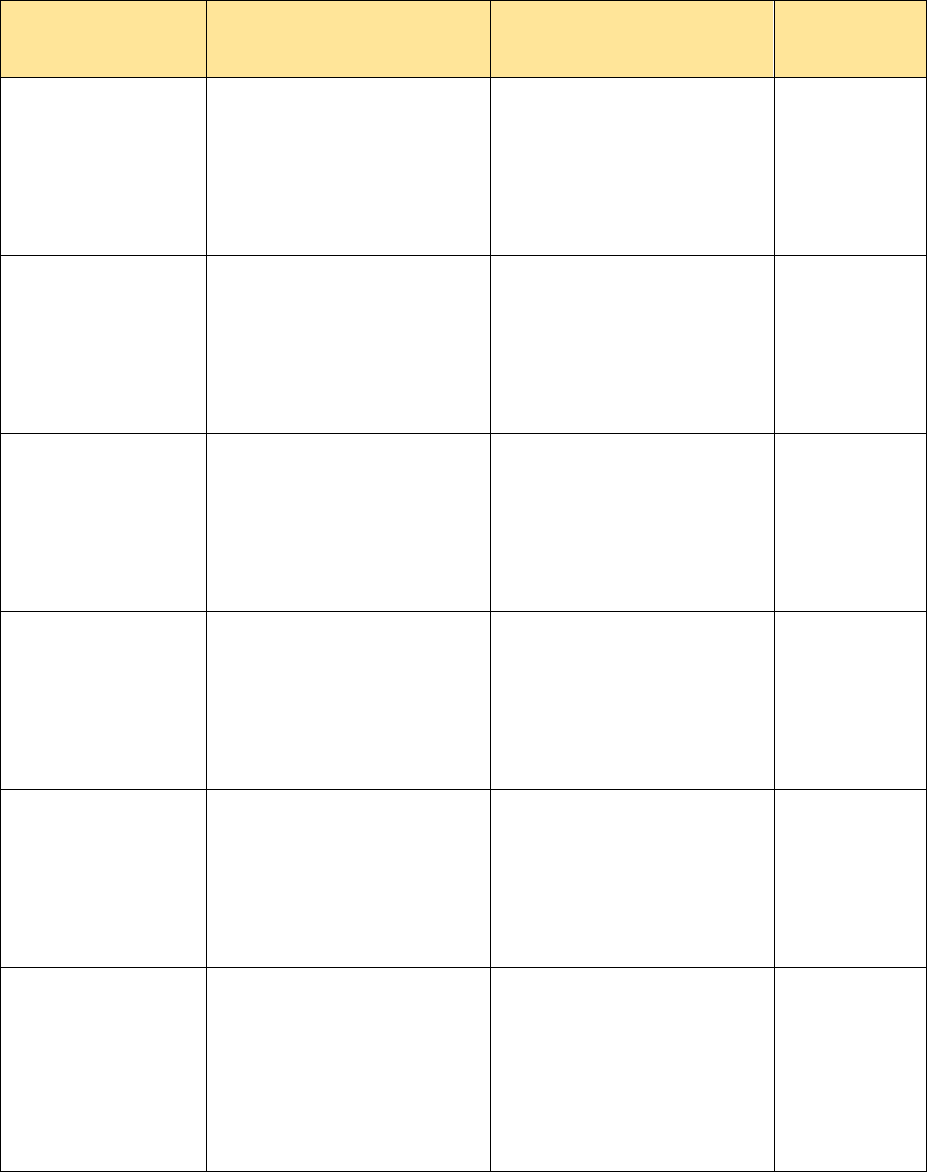
Page 49 of 72
Appendix B: ASAM Criteria Dimensions and Rationale Worksheet
ASAM Criteria
Justification (diagnosis)
Justification (ASAM
severity based on
impairments)
Severity/ Risk
Rating
Dimension 1: Acute
Intoxication and/or
Withdrawal
Potential
Dimension 2:
Biomedical
Conditions and
Complications
Dimension 3:
Emotional,
Behavioral, or
Cognitive
Conditions and
Complications
Dimension 4:
Readiness to
Change
Dimension 5:
Relapse, Continued
Use, or Continued
Problem Potential
Dimension 6:
Recovery/Living
Environment

Page 50 of 72
Appendix C: Documenting Impairments Related to SUD Guide
Think about what it is about the client’s use of substance(s) that makes them take a particular action,
which results in a significant impairment in an important area of life functioning.
FORMULA:
Due to client’s __________________ (symptoms of SUD), client __________________ (behaviors)
resulting in ____________________________ (impairment).
Example: “Due to client’s dependency on sustaining his meth use, client attempted to sell a car he stole,
resulting in his arrest, incarceration, and current probation status.”
*NOTE: It is not required or necessary to use this formula…as long as the documentation shows how all three are
connected, you can write it however you like!
Pro Tip:
If you know the impairment (unemployment, no housing, loss of social support, etc.), you can work backwards to
get to the behavior and how it is related to a SUD.
Example: Client has been unemployed for the past 3 years.
Q: What happened 3 years ago with his/her employment?
A: He/she lost his/her job.
Q: How did he/she lose their job?
A: He/she was fired.
Q: What did he/she do that got him/her fired?
A: He/she stopped showing up for work.
Q: Why did he/she stop showing up for work?
A: He/she was drinking throughout the night and unable to get up in the morning. He/she started showing up to
work later and later, eventually stopping. He/she has not been able to work since then.
Due to client’s excessive drinking throughout the night, he/she was often tardy or did not show up to work because
he/she was unable to get up in the morning, which resulted in him/her getting fired and being unemployed for the
past 3 years.
Symptom of SUD Behavior Impairment

Page 51 of 72
Appendix D: What Needs to be in The Case Formulation?
1. Basis for the DSM-5 SUD diagnosis description of how the client meets criteria for the
diagnosis
2. Impairments related to the SUD description of life areas most severely affected by the
substance use
3. Corresponding level of care what is indicated based on 1 and severity of 2 that will meet the
client’s needs
Sample Format:
“Client meets criteria for _________________________ (DSM-5 SUD diagnosis). Severity is
_______________ (mild, moderate, severe) as he/she meets ____________ (number of DSM-5
criteria for SUD diagnosis) of the criteria. Client endorses ___________________________
(criteria). (Continue with all criteria). Client has had a pattern of problematic use over/within
the last ___________ (duration of use).
Client meets medical necessity based on the above diagnosis and significant impairment in
dimensions ____________ (numbers with most severe risk ratings) of the ASAM Criteria. Due to
client’s ____________ (symptoms of SUD), client _____________________ (behaviors) resulting
in ______________________ (impairment). (Continue with other dimensions with the most
severe risk ratings). Client is most appropriate for _____________________ (level of care) and
will need _____________ (services that will address client’s problems).”
**Any format can be used, as long as the required elements are addressed!**
Example:
Client meets criteria for (F10.10) Alcohol Use Disorder, Moderate. Severity is moderate as she meets 5
of the criteria. Client endorses daily cravings to use that have led to preoccupation with drinking and
feelings of agitation and restlessness. Client states that she has stopped working out and spending time
with friends and family. She spends most of her time at home drinking alone, often neglecting to take
care of responsibilities like paying bills and completing household tasks. Client stopped going to her job
as a waitress because she was either drinking at home or sleeping after blacking out. Client has had a
pattern of problematic use over the last year, but client has been sober for about two weeks.
Client meets medical necessity based on the above diagnosis and impairment in dimensions 5 and 6 of the
ASAM Criteria. Due to client’s inability to tolerate cravings to continue drinking, client states she is
“always planning my next drink” and has stopped participating in social activities with friends and family.
Client states that she feels guilty for this and that she would like to be close with her family again and
“have people that are there for me instead of being all alone because I pushed everyone away.” Due to
client spending time drinking, she has not been keeping up with paying bills or completing household
tasks, resulting in her being behind on payments and accumulating debt. She is no longer able to pay off
the debt because she has no job. Due to her spending time drinking or recovering from the effects, client
has stopped going to work resulting in job loss. Client’s risk for continued use and problem potential are
significant as she states that she has not made any attempts to try stopping since she began and that “I
don’t know how to stop.” Client was unable to verbalize any ways to manage cravings, other than by
drinking, and states that “everything is a trigger.” Therefore, client does not have the skills needed to be
able to abstain from drinking for prolonged periods of time. Client would benefit most from the Intensive
Outpatient Treatment Services level of care to increase her understanding and awareness of the effects of
drinking as well as cravings and triggers. Client needs a moderate level of support to be able to learn
Page 52 of 72
healthy coping skills and relapse prevention skills in order to become self-sufficient in applying them as
she improves in functioning.

Page 53 of 72
Appendix E: Billing Assessment and Re-Assessment Activities

Page 54 of 72

Page 55 of 72
Appendix F: Treatment Plan Reference Sheet
How do I know what goals to create?
1. Ask the client what he/she wants or needs the most help with!
2. Look at the dimensions of the ASAM Criteria and find the highest risk level ratings.
3. Discuss with client what he/she would like to improve in each dimension.
STATEMENT OF PROBLEM:
1. In the client’s own words. Can use quotes.
2. Can be long-term.
3. May or may not be achievable during this treatment phase.
4. Should tie back to the impairments identified in the assessment (making it related to
SUD).
5. OK if it does not directly relate to SUD. **If it does not relate to SUD, explore with
client to break it down to what can be worked on in the short-term!**
STATEMENT OF GOAL:
1. This is what will help the client work towards resolving the statement of the problem
above.
2. Must relate to SUD.
3. Must be SMART.
a. Specific
b. Measurable
c. Achievable
d. Realistic
e. Time-bound
4. Duration (how long will it be worked on for? i.e., For the next 30 days, 90 days, etc.)
ACTION STEPS:
1. Describes what you as the provider will do to help the client meet his/her goal above.
2. Describes what the client will do to work towards his/her goal above.
3. Must include-
a. who will provide the service (i.e., counselor, provider, therapist, etc.)
b. type of service (i.e., individual counseling, group counseling, case management)
c. frequency (how often? i.e., 1x/week, 2x/month, etc.)
TARGET DATE:
1. The expected date that client will achieve his/her action steps above.
2. Not program specific (i.e. date of discharge after the 8 week program).
3. Can be before the discharge date. All action steps of a goal may have the same target
date.

Page 56 of 72
STATEMENT OF PROBLEM
STATEMENT OF
GOAL/OBJECTIVE
ACTION
STEPS

Page 57 of 72
Appendix F: What are SMART goals?
o Related to the problem
o Clearly ties back to the SUD
o Concrete
o Action verbs
Sample formula – “Client will _____________ (action verb)…”
Example – “Client will use healthy coping skills to manage triggers…”
o There is a baseline and target
o Quantifiable
o Observable
o Behaviors
Sample formula – “from __________ (baseline) to ______________ (target)…”
Example – “…from 0x/day to 3x/day…”
o Can be done in this level of care
o It is appropriate for this level of care
o It is appropriate to the client’s needs and abilities
o Can reasonably expect that client can meet this goal
o Set up for success!
o A set timeframe for when client will be able to meet this goal
o Set amount of time for monitoring progress
Sample formula – “…in the next _____________ (timeframe).”
Example – “…in the next 30 days.”
SAMPLE FORMULA: “In the next _________ (timeframe), client will
____________________ (behavior change) from ________ to __________
(baseline and target) in order to _____________ (problem).”
Page 58 of 72
Appendix G: Treatment Plan Checklist
Statement of Problems
☐
Can be i
n the client’s own words
☐ Tied back to the ASAM dimensions
Statement of the Goal
☐
Specific
☐ Related to SUD
☐ Ties back to the problem identified in the ASAM Dimension
☐
Measurable
☐
Achievable
☐
Realistic
☐
Time-Bound
Action steps & Target Date
☐
Each indicates the type of service
☐
Each includes the frequency
☐
Written as what client or counselor will do (either or both)
☐
Connected to the goal/objective
☐
Reasonable expectation that this will help the client
☐
Within the scope of practice for the counselor
☐
Target date is indicated for each action step
Signatures
☐
Signature line includes printed name and credentials
☐
Signed by the counselor
☐
Counselor signature has the date of signature
☐
Signed by client
☐
Client signature has the date of signature
☐
If client has refused to sign, it is documented (along with plan for how to address this) in the
progress note
☐
Signed by the Medical Director/physician or LPHA
☐
Medical Director/physician or LPHA signature has the date of signature

Page 59 of 72
Appendix H: Sample Treatment Plan

Page 60 of 72

Page 61 of 72

Page 62 of 72
Appendix I: Sample SUD Re-Assessment (Continuing Services Justification)

Page 63 of 72

Page 64 of 72

Page 65 of 72

Page 66 of 72

Page 67 of 72
Appendix J: SUD Progress Note Checklist
Format:
GIRP
Goal
Intervention
Response
Plan
Requirements:
Date of session
Start/End time of session
Start/End time of documentation minutes
Location (or indicate by telephone or telehealth if not face-to-face)
If session is conducted out in the community, there must be documentation of how confidentiality
was ensured in that location.
Type of service
Topic or purpose of session
Client’s progress towards treatment plan goals (in the Plan)
Counselor’s printed name and credentials, signature, and date (date of documentation)
Note written and signed within 7 days of date of service
If more than 7 days: note must be made non-compliant

Page 68 of 72
Appendix K: Progress Note Elements
IS THIS BILLABLE, NON-BILLABLE, OR NON-COMPLIANT?
HOW DO I DETERMINE TIME SPENT ON AN ACTIVITY?
Face-to-Face time
Time with the client, in person.
Non-Face-to-Face time
Billable or non-billable time spent on a service activity that does not include
interaction with the client.
Example: Analyzing information to determine risk rating levels for the
dimensions of the ASAM Criteria outside of the session with client. The time
spent working on this is billable.
Service Minutes
The combination of time spent face-to-face with a client in session and/or any
billable non-face-to-face time.
Documentation Minutes
Time it took to complete the progress note. This should never exceed the
length of the session and should correspond to what is reasonable in
comparison to what is written. Working on any other documents besides the
progress note is not considered documentation time.
Travel Minutes
Time it takes to travel from one location to another to meet with client or
provide a service. Transporting a client does not count for this. If solely
transporting a client from point A to point B, this time is non-billable (Medi-
Cal will not reimburse for us being a taxi service).
If during the course of transporting the client from point A to point B, some
service is provided (such as discussing recent response to triggers and use of
coping skills), the portion of the time that is spent counseling is considered
Service Time because you provided a service. This does not mean that if 5
minutes of counseling was provided during a 30 minute drive, we can bill all
30 minutes! Only the time spent providing an actual service can be billed.
BILLABLE
NON-BILLABLE
NON-COMPLIANT
What Medi-Cal will pay for.
What Medi-Cal would NEVER pay
for.
What Medi-Cal could have paid for,
but we did something wrong.
Examples:
• Correct code to type of
service provided
• Interventions address SUD
and meets medical necessity
• Within scope of practice of
the counselor
Examples:
• Clerical
• Solely social/recreational/
vocational
• Unrelated to SUD and no
medical necessity established
Examples:
• Two types of services
provided under one code
(blended)
• Out of the timeframe
• Out of scope of practice of
the counselor

Page 69 of 72
Appendix L: Documentation Language by Service Type
INDIVIDUAL/GROUP COUNSELING:
Assessment:
Tx Planning:
Crisis:
Individual/family/group:
Collateral:
DC Planning:
Asked
Assessed
Ascertained
Attempted
Clarified
Determined
Developed
Elicited
Evaluated
Explored
Formulated
Gathered
Gauged
Inquired
Obtained
information
about…
Probed
Questioned
Reviewed
Synthesized
Analyzed
Created
Developed
Established
Formed
Formulated
Generated
Produced
Synthesized
Assessed
Assisted
Attempted
Coordinated
De-escalated
Empathized
Empowered
Ensured
Evaluated
Facilitated
Focused on
Fostered
Helped
Intervened
Monitored for
Obtained
Offered
Promoted
Provided
Reassured
Recommended
Responded to
Stabilized
Supported
Showed
Acknowledged Redirected
Assisted Reinforced
Attempted Reiterated
Challenged Reviewed
Coached Role played
Discussed Shared
Demonstrated Supported
Described Showed
Empathized Taught
Educated Validated
Elicited Verbalized
Empowered
Encouraged
Engaged
Explained
Explored
Expressed
Fostered
Helped
Introduced
Inquired
Maintained
Modeled
Motivated
Normalized
Offered
Practiced
Processed
Prompted
Promoted
Provided
Recommended
Consulted
Collaborated
Coordinated
Shared
Exchanged
Discussed
Reviewed
Prepared for
Planned
Developed
Inquired
Asked
Questioned
Followed up
Elicited
Developed
Discussed
Explored
Reviewed
Formulated
Established
Set
Prepared
Revised
Coordinated
Collaborated
CASE MANAGEMENT:
Advised
Collaborated
with
Devised
Followed up
Inquired
Referred
Aided
Communicated
Directed
Furnished
Instructed
Reinforced
Answered
Connected
Discussed
Guided
Linked
Reminded
Arranged
Consulted
Educated
Helped
Offered
Reviewed
Assigned task
Contacted
Encouraged
Helped plan
Planned
Set up
Assisted
Coordinated
Explained
Highlighted
Prepared
Suggested
Attempted
Demonstrated
Explored options
Identified
Provided
Talked about
Checked in
Developed
Facilitated
Informed
Recommended
Worked on

Page 70 of 72
Appendix M: Sample Discharge Plan
Today’s Date:
10/12/17
Admission Date:
9/29/17
Planned Discharge Date:
12/28/17
Name:
Doe, Joe
Current Level of Care:
Intensive Outpatient Treatment
My Counselor’s Name: Mary Sunshine, CADC II Contact: (714) 987-6543
Why I Want To Stay Sober:
“I want to go back to being like how I was before the accident.”
My Treatment Goals:
1. To get help for my back pain
2. Learn how to deal with triggers and cravings
3. Go back to working
My Relapse Triggers:
1. Back pain
2. Not having a job
3. Not having own place to live
4. Conflict with family
Things I Can Do When I Get Triggered:
1. Deep breathing, meditation
2. Positive self-talk (remind myself that I am
working towards it), go to a meeting
3. Positive self-talk (remind myself that I am
working towards it), making a gratitude list, go to
a meeting
4. Talking to my sponsor, go to a meeting, listen
to music
SUPPORT PLAN:
People I Can Contact For Support When I Get Triggered:
1. Name: David Goodguy Relationship: Sponsor Contact: (310) 222-1515
2. Name: James Peach Relationship: Friend Contact: (714) 111-2323
3. Name: ____________________ Relationship: ____________ Contact: ____________
Community Resources I Can Access For Support:
1. Name of Organization: OC Narcotics Anonymous Contact: (714) 590-2388
Address: __________________________________________________________________
2. Name of Organization: First United Methodist Church Contact: (714) 542-2322
Address: 609 N. Spurgeon St., Santa Ana, CA 92701
3. Name of Organization: Orange County Rescue Mission Contact: (714) 247-4300
Address: 1 Hope Drive, Tustin, CA 92782
Additional Resources To Help Me With My Treatment Goals:
1. Name of Organization: One-Stop Center, Santa Ana Contact: (714) 565-2600
Address: 1000 E. Santa Ana Blvd., Ste. 200, Santa Ana, CA 92701
2. Name of Organization: Orange County Housing Authority Contact: (714) 480-2700
Address: 1770 N. Broadway, Santa Ana, CA 92706
3. Name of Organization: ________________________________ Contact: ____________
Address: __________________________________________________________________
Client’s Name: _____________________ Signature: _____________________ Date: __________
Counselor’s Name: Mary Sunshine, CADC II Signature: _____________________ Date: __________
Copy of Discharge Plan provided to client; if no, provide reason: __________________________________________________________________________

Page 71 of 72
Appendix N: Sample Discharge Summary

Page 72 of 72
